Table of Contents
Introduction
The body is held up by skeletal joints that keep the body upright and provide everyday movements for the body to go anywhere at any time. The musculoskeletal system provides the muscles, tissues, and ligaments that encase the skeletal joints protecting them from unknown factors that can cause harm to the body. The internal organs also have a purpose in the body as they help provide the nutrients and necessary hormones to the muscles and joints that need these nutrients to function. When environmental factors affect the body, either internal or external, it can cause the body to become dysfunctional and even cause unwanted symptoms that affect the internal organs that correspond to the muscles suffering. Today’s article looks at pelvic pain, how gut disorders are associated with pelvic pain, and how viscerosomatic pain affects the pelvis. We refer patients to certified, skilled providers specializing in osteopathic and gut treatments that help those with gut disorders and pelvic pain issues. We also guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is critical for asking insightful questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
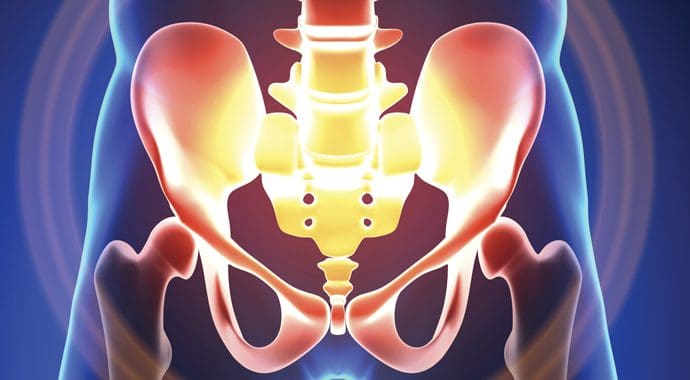
What Is Pelvic Pain?
Have you been experiencing gut issues that are affecting your pelvic region? Has your gut been feeling inflammatory effects? Have you noticed that you need to go to the bathroom more frequently than usual? Many of these symptoms are some of the signs that are associated with pelvic pain. Research studies have defined pelvic pain as disabling, chronic, and persistent pain that commonly affects women. Pelvic pain can range from acute to chronic depending on how severe the pain affects the pelvic region of the body. Additional research studies have mentioned that pelvic pain in its chronic form can become a multifactorial disorder that can cause pain in the gastrointestinal, pelvic musculoskeletal, or nervous system, making the immune, neurological, and endocrine metabolism dysfunctional. When pelvic pain begins to affect the gastrointestinal system, it can lead to various gut disorders that can cause the pain to become worse if it is not treated.
How Do Gut Disorders Associate Pelvic Pain?
Research studies have mentioned that since pelvic pain is a multifactorial disorder, it can cause pain to arise in the internal organs in the gastrointestinal system. When pelvic pain starts to affect the gastrointestinal system, it can cause the development of gut disorders to affect the body further. When gut disorders co-exist with pelvic pain, it can cause an enhancement to the overall pain symptoms that are becoming the result of viscerosomatic dysfunction through the cross-organ sensitization mechanisms. Additional information studies have mentioned that gut disorders like IBS (irritable bowel syndrome) can cause changes in thermal/visceral pain sensitivity that overlap in the lower body’s pelvic region, further enhancing rectal/thermal pain. This can cause a person to become miserable and even affect their quality of life since they are suffering from so much pain.
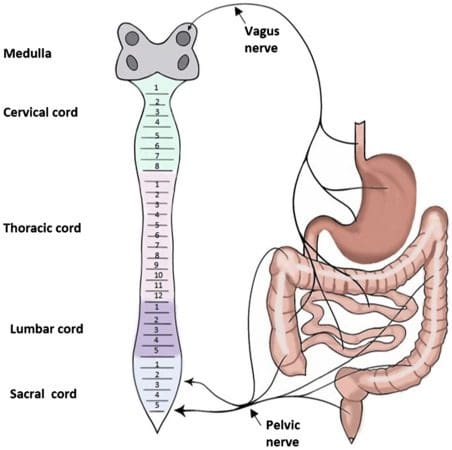
Visceral Afferent Nerves Being Affected By Pelvic Pain-Video
Have you experienced gut issues like IBS (irritable bowel syndrome), inflammation, or IBD (inflammatory bowel disease)? Have you felt pain in your pelvic region constantly? Has the pain-affected certain areas in your body, not just your pelvis? If you have these symptoms, it might be due to your visceral nerves being involved. The video above explains what the visceral afferent nerves from the pelvic region are doing to keep the body functioning in the lower extremities. The visceral afferent nerves become aggravated by environmental factors affecting the body, including the gut system. Symptoms of inflammation and gut disorders from persistent aspects of many forms of stress or trauma can cause visceral pain to affect the body, thus causing pelvic pain, gut issues, lower back pain, and other body pains.
How Viscerosomatic Pain Affects The Pelvis
The body’s viscerosomatic pain can be complex since the organs also affect the corresponding muscles. The way the pain is described in the body from viscerosomatic pain ranges from dull to excruciating pain. Research studies have mentioned that the burden of viscerosomatic pain emanates from the internal thoracic, pelvic, and abdominal organs associated with the muscles. For visceral pain to affect the pelvic region, research studies have shown that the nociceptive pain from the pelvic area is usually visceral from the results from the pelvic organs that are poorly localized and can overlap with the somatic sensory tracts that are located in the spinal cord. When this happens, it can cause significant discomfort to the pelvic organs in the body and affect the individual with excruciating painful symptoms.
Conclusion
The body provides everyday movements held by the skeletal joints that help the body go anywhere. While the musculoskeletal system and the internal organs help give the muscles, tissues, ligaments, and nutrients the body needs to function. When environmental factors affect the body, it can lead to various issues that cause gut disorders and even pain in the pelvic region, known as visceral pain. Visceral pain is a complex disorder since the affected organs also affect the corresponding muscles. For visceral pain to affect the pelvic area, it can lead to dull excruciating pain in the pelvic organs and affect the individual. Visceral pain can also overlap the sensory somatic tracts in the spinal cord, causing unbearable painful symptoms to the body while inflammatory issues in the gut system are developing. When people realize that the pain is affecting them, they can start to find treatments from their specialized providers to help alleviate their pain.
References
Dydyk, Alexander M, and Nishant Gupta. “Chronic Pelvic Pain – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 11 Nov. 2021, https://www.ncbi.nlm.nih.gov/books/NBK554585/.
Grinberg, Keren, et al. “New Insights about Chronic Pelvic Pain Syndrome (CPPS).” International Journal of Environmental Research and Public Health, MDPI, 26 Apr. 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7246747/.
Origoni, Massimo, et al. “Neurobiological Mechanisms of Pelvic Pain.” BioMed Research International, Hindawi Publishing Corporation, 2014, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4119661.
Udoji, Mercy A, and Timothy J Ness. “New Directions in the Treatment of Pelvic Pain.” Pain Management, U.S. National Library of Medicine, Sept. 2013, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3979473/.
Verne, G Nicholas, et al. “Viscerosomatic Facilitation in a Subset of IBS Patients, an Effect Mediated by N-Methyl-D-Aspartate Receptors.” The Journal of Pain, U.S. National Library of Medicine, Sept. 2012, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3489925/.
Yuan, Tian, and Beverley Greenwood-Van Meerveld. “Abdominal and Pelvic Pain: Current Challenges and Future Opportunities.” Frontiers in Pain Research (Lausanne, Switzerland), Frontiers Media S.A., 4 Feb. 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8915637/.
Disclaimer
General Disclaimer
Professional Scope of Practice *
The information herein on "The Connection Between Gut Issues & Pelvic Pain" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics