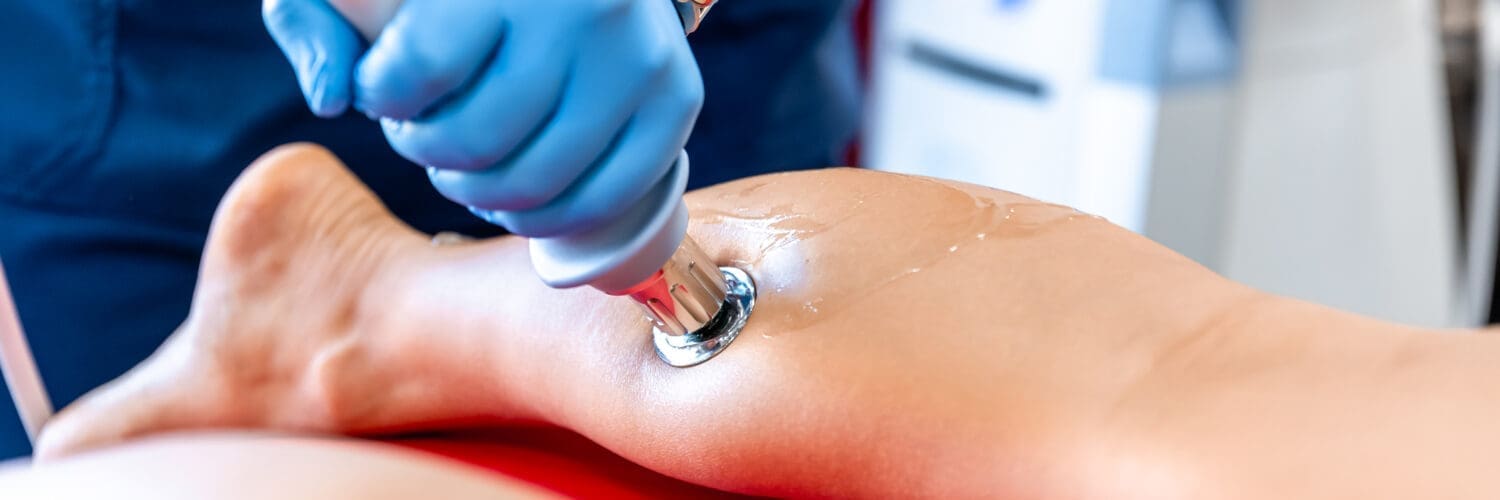
Learn about the innovative therapeutic approaches of photobiomodulation for tissue regeneration for improved tissue healing.
Table of Contents
Abstract: A Clinician’s Field Guide to Advanced MLS Laser Therapy for Spine, Joint, and Soft-Tissue Care—Dosing, Physiology, and Practical Protocols from the Exam Room
I’m Dr. Alexander Jimenez, DC, FNP-APRN. In this educational post, I synthesize cutting-edge findings from leading researchers in photobiomodulation and present how I apply these insights at the point of care. My goal is to bridge scientific rigor with real-world clinical utility so you can understand how to dose, target, and combine multiwavelength laser therapy—specifically MLS-class systems using 808 nm and 905 nm—in an evidence-informed, patient-centered fashion. I also integrate my clinical observations and protocols refined across years of musculoskeletal, neuropathic, sports, and orthobiologic collaboration. For additional context on my approach, you can explore related clinical observations at HealthVoice360.
The discussion unfolds in six layers. First, I outline how I prioritize patient comfort, positioning, and safety to achieve reproducible outcomes—especially when using automated robotic heads. Second, I detail the operational logic of area targeting using X–Y coordinates and precision spacing for beam collimation, explaining why correct standoff distances and skin-contact vs non-contact delivery materially change the dose, depth, and patient sensation. Third, I delve into dosing theory: why we dose in energy density (J/cm²) rather than in raw joules, how we avoid “overcooking” tissue (bioinhibition), and how software that auto-recalculates the dose based on the treatment area improves fidelity and safety.
Fourth, I explore mechanisms and timelines: fast-acting nociceptive modulation; hemodynamic and neuroimmune shifts that calm peripheral and central sensitization; and mitochondrial photobiology that remodels cellular energetics and redox signaling over days to weeks. I map these effects to clinical milestones—what patients may feel at 4–6 hours, at treatment 3–5, and after 6–12 sessions—and explain the logic behind treatment schedules for acute vs chronic conditions. Fifth, I address integration with orthobiologics (e.g., PRP): how pre-, day-of-, and post-injection laser sessions “prep the soil,” augment pro-inflammatory priming, and support post-injection integration without blunting desired inflammatory cascades. I also describe synergy with neuromuscular rehab, shockwave therapy, and adjunct mitochondrial supports (e.g., sleep, nutrition, and selected nutraceuticals) to optimize outcomes, while highlighting safety and scope boundaries.
Sixth, I provide condition-specific playbooks—including low-back pain with facet involvement, knee osteoarthritis, plantar fasciitis, peripheral neuropathic pain, post-surgical scenarios, and select fracture-healing considerations—defining target areas, patient positioning, typical energy-density windows (often 4–10 J/cm²), session counts, and technique selections (robotic head vs handpiece vs hybrid). I discuss what patients do and do not feel; how to use phones to visualize the 808 nm beam footprint; and why short, high-peak 905 nm pulses help maintain a steady tissue temperature by allowing rest periods between absorption events.
Throughout, I present why each parameter matters: wavelength selection and pulse structure, power density, treatment geometry, and temporal sequence. I compare contact and non-contact delivery using diodes and optics, and explain how to tune your field size to treat the primary pathology and contiguous fascial and neural corridors—the clinical multimodal approach. I describe why posterior and posteromedial windows are often necessary around joints (e.g., the knee) to bypass reflective interfaces, such as the patella, and safely access posterior capsular and neurovascular structures. I also share how to avoid common pitfalls: chasing pain without addressing source drivers; overdosing a single zone rather than distributing dose across anterior–posterior or medial–lateral windows; and stopping at “feels better” after 3–5 sessions instead of completing a 6–12 protocol that consolidates gains.
In later sections, I unpack the physiology in depth: chromophore targeting (cytochrome c oxidase, transient receptor potential channels, heme proteins), nitric oxide dynamics, ATP upregulation with controlled ROS signaling, lymphatic flux, fibroblast/tenocyte responses, nociceptor gating, microglial modulation, and matrix remodeling timelines. I translate these into clear treatment logic: rapid pain relief mechanisms, subacute vascular-immune normalization, and long-horizon bioenergetic and connective-tissue remodeling. For orthobiologics, I discuss how pulse-structured dual-wavelength MLS interacts with PRP’s inflammatory-to-anabolic trajectory and outline parameter strategies that support, rather than suppress, regenerative intent.
Finally, I detail program design: scheduling (e.g., M–W–F to 6 or 12 treatments), package structuring to improve adherence, post-session behavioral guidance, and documentation strategies that track pain, function, load tolerance, and quality-of-life measures. I include Q&A-inspired expansions on fracture care timing (noting off-label considerations), thermal vs non-thermal effects, device reliability, service networks, and how auto-dosing by adjusted X–Y fields reduces human error. By the end, you will have a comprehensive blueprint for implementing modern MLS laser therapy with methodological rigor, physiological depth, and patient-centered practicality.
Keywords in this post are bolded and highlighted to help you locate key concepts. Each conceptual area is presented with a search-optimized heading. The full text offers a comprehensive, narrative-based explanation intended for clinicians who want to understand both the “how” and the “why” of laser therapy—so you can integrate it intelligently with other modalities and match your dosing and protocols to the biology you aim to influence.
Patient-Centered Setup and Comfort: Foundations for Reproducible Laser Care
In my practice, patient comfort is non-negotiable. Whenever I position an MLS robotic laser over the low back—or any region—I think in terms of three pillars:
- Comfort and immobility
- Precision alignment
- Reliable dosing
When a patient lies prone for low-back care, I ensure the table supports the pelvis and thorax without undue pressure on the abdomen, as this can subtly alter lumbar lordosis and shift the target zone. Because the robot relies on precise placement within a defined X–Y field, I want the patient to be relaxed and still. A restless patient—even a few millimeters of drift—can compromise treatment fidelity. If I know I’ll step away for workflow reasons, comfort becomes even more critical.
Skin contact vs non-contact matters. With the handheld diode, I typically use direct skin contact for trigger points and joint spaces, and dynamic maneuvers (e.g., light range of motion during therapy). With the robotic head, the optics are designed for a specific standoff distance—about 5–7 inches, with a 6-inch “sweet spot”—to maintain a collimated beam and predictable energy density. The supplied ruler is not a gimmick; it is a dose instrument. Collimation affects spot size, power density, and ultimately the therapeutic dose reaching deeper tissues.

When patients ask what they should feel, I explain: with MLS dual-wavelength, high-peak, short-pulse design, they often feel nothing, occasionally a faint warmth or tingling. If sensitive patients report sensation, I reassure them that the system’s pulse timing includes off periods that allow energy absorption while keeping surface temperatures stable. The absence of heat does not mean absence of effect; MLS therapy’s physiology is driven primarily by photochemical and photophysical signaling, not bulk thermal loading.
Precision Targeting with X–Y Fields: From Pain Site to Source and Surround
I center the robot over the area most consistent with the patient’s dominant pain generator—say, the right L4–L5 facet complex with referred ache into the right paraspinals. I zero the X and Y axes, align with the “epicenter,” and then expand the field to encompass clinical reality: structures do not operate in isolation. I teach my teams to cover not only the painful locus but also the connective tissue corridors—fascia, paraspinal muscle bands, and segmental ligaments—thereby creating a more comprehensive therapeutic field.
This is my clinical multimodal approach within the laser session itself. Rather than “chasing pain,” I target the architectural context: regions of guarded tone, taut bands, lateral shift in fascia, and neurovascular tracks that may perpetuate nociceptive input. The robot’s software recalculates time automatically when I enlarge or shrink the X–Y field to deliver the prescribed energy density—this reduces human error and maintains dosing integrity. When I add the handheld diode to address punctual trigger points, I match the density to the target’s size and depth. For discrete trigger points, 20–40 seconds per spot is often sufficient within an overall session that may run 6–12 minutes on the robot for a back region.
Patients enjoy seeing the 808 nm “triangle” via their smartphone cameras—a quick educational visual. The camera captures the 808 nm continuous/longer-pulse component, while the 905 nm pulsed emission may be invisible due to its pulsed characteristics. That triangle roughly marks the active footprint, not the broader red glow; understanding this helps patients grasp why remaining still matters.
Contact vs Non-Contact: When Each Matters and Why
- Handpiece (contact): I prefer direct skin contact for focal work—trigger points, joint lines, small tendinopathies—where tactile feedback and subtle motion can “milk” fascial planes, recruit sliding surfaces, and build patient confidence through movement exposure. Contact delivery minimizes air gaps and reflective loss, allowing efficient dosing of small targets.
- Robotic head (non-contact): The robotic system, with three diodes and collimated optics, is designed to sit off the body at a precise standoff distance. It excels for broader fields, non-contact needs (hypersensitivity, post-surgical sites, tactile-avoidant patients), and standardized reproducibility across sessions and staff. This is invaluable in busy practices and research-grade protocols.
- Hybrid approach: In many sessions, I run the robot over a defined X–Y field while I simultaneously address satellite trigger points or distal contributors (e.g., gluteal trigger points during low-back sessions) with the handheld. Both run on separate channels. This two-channel workflow is efficient and leverages the strengths of both delivery modes.
Power, Pulse, and Temperature Stability: The Physiology of “Feeling Nothing”
MLS systems pair an 808 nm wavelength with a 905 nm high-peak pulsed beam—often citing up to 50 W peak in the pulsed channel. The “secret sauce” is high peak power in micro- to millisecond bursts, with duty cycles that allow tissue to absorb photons without accumulating heat. That is why, even at peak powers as high as 1000 W, patients rarely feel warmth; surface temperature remains largely stable over time.
This matters physiologically and practically:
- Thermal neutrality preserves comfort and safety.
- Pulsed 905 nm improves depth reach and photon delivery efficiency without cooking the surface.
- Off periods allow oxygen, hemoglobin, and chromophores to reset binding states, facilitating sustained photochemical signaling rather than thermal denaturation.
If you feel heat at the surface with any laser, you may be using a different wavelength mix, an overly high continuous-wave output, or a dose that the tissue cannot absorb at that rate. The MLS pulse pattern is engineered to avoid that, while still delivering robust energy densities to deeper targets.
Dose Is Energy Density: Why J/cm² Beats “Total Joules”
I teach teams to dose to a target energy density—often 4–10 J/cm² for many musculoskeletal and neuropathic indications—rather than chasing a raw joule total. The tissue responds to the density delivered per unit area, not the grand sum smeared across poorly defined fields. The World Association for Laser Therapy (WALT) and broad photobiomodulation literature emphasize joules per square centimeter as the meaningful “dose.”
- Typical therapeutic window: 4–10 J/cm², adjustable by condition and acuity.
- Example: For a facet-dominant low back with right-sided involvement, I may select 6 J/cm² across a tailored X–Y field that encompasses the facets, paraspinals, and fascia; automated software will set the time to achieve that density in that area.
Bioinhibition is real. The Arndt–Schulz principle reminds us that too little energy may be inert, while too much can suppress or delay beneficial responses. Rather than piling all doses into a single anterior knee window, for example, I distribute density across anterior, medial, and posterior fields to cover the joint capsule and periarticular tissues without saturating any one area. If a patient requests “more time,” I prefer to add windows (e.g., posterior knee) rather than stacking redundant dose on one surface.
What Patients Feel and When: 4–6 Hours, 3–5 Sessions, and 6–12 Sessions
- Within 4–6 hours: Many patients report a first wave of relief—often interpreted as nociceptive gating, reduced peripheral input, and microvascular shifts reducing local irritability. I ask them to self-test familiar pain-provoking tasks later the same day and report back.
- After 3–5 sessions, we often see consolidation—less morning stiffness, improved motion arcs, decreased protective guarding, and better load tolerance. This is likely due to cumulative changes in microvascular, neuroimmune, and peripheral/central sensitization.
- By 6–12 sessions, we expect function-level gains in walking speed/distance, sit-to-stand ease, tolerance to rehab loading, sleep quality, and decreased flare frequency. This window aligns with deeper connective-tissue remodeling and mitochondrial gains that require repetition and time to manifest.
I do not promise miracles in one visit. I set expectations around a series—”effects are cumulative”—and I strongly encourage completing the protocol even if relief appears early. Stopping at session 3 often results in long-term losses.
Acute vs Chronic Scheduling: Protocol Logic
- Acute conditions: 6 sessions are a strong starting point. If logistics allow, daily or every 24 hours is ideal early on to capture momentum. Realistically, three times weekly (e.g., Monday–Wednesday–Friday) works well, reaching six visits in ~2 weeks.
- Chronic conditions: 12 sessions create a robust base. Same scheduling—three per week—yields about four weeks to completion. Many chronic patients “feel” changes by sessions 3–5; I explain why we keep going to consolidate neuroimmune and connective-tissue remodeling.
I typically bundle care into packages to support adherence. You do not need to collect the full program cost upfront, but packaging clarifies expectations and protects the patient from the common pitfall of stopping early.
Low Back Pain with Facet Involvement: My Targeting Blueprint
For a patient describing axial low-back pain with stiffness and suspected facet contributions at L4–L5 (and perhaps L5–S1), often with mild referral into ipsilateral paraspinals:
- Position: Prone, pelvis and thorax comfortably supported. Encourage stillness.
- Robot field: Zero X–Y on the epicenter of pain; expand to include ipsilateral paraspinals, multifidus corridor, and relevant fascia. Prescribe 6–8 J/cm² depending on acuity and tolerance.
- Handpiece augmentation: Palpate “cooked meat” nodules—the firm, fibrotic, tender bands—and apply focal contact dosing 20–40 seconds per spot at a matched density. Combine with slow diaphragmatic breaths to downshift sympathetic tone.
- Session length: 6–10 minutes robotic field; add 2–4 minutes handheld focal work.
- Schedule: Acute—6 sessions; Chronic—12 sessions; M–W–F cadence works well.
- Expectations: Little to no heat sensation; some feel subtle tingling. Ask for a function check 4–6 hours later (e.g., sit-to-stand, forward bend, walk).
- Rationale: We’re addressing not only facet nociception but also paraspinal hypertonicity, fascial shear, and microvascular congestion—all of which perpetuate pain. Dual-wavelength MLS supports rapid nociceptive modulation, hemodynamic normalization, and—over the course of sessions—myofascial and mitochondrial remodeling.
Knee Osteoarthritis: Multiplanar Windows, Not Just Anterior
For knee OA, direct anterior-only dosing risks energy reflection off the patella and reduced intra-articular reach.
- Position: Supine with knee flexed ~20–30 degrees supported by a bolster to open the joint space. Consider posterior access in the prone or side-lying position for the posterior capsule, popliteal region, and neurovascular corridor.
- Windows:
-
- Anterior-medial: Target the medial joint line, MCL/femoral condyle interface, and pes anserinus tendinopathy if present.
- Lateral: If lateral compartment disease or iliotibial band irritation.
- Posterior: Popliteal fossa, posterior capsule to reach the inflamed synovium and posterior horn meniscal irritation.
- Energy density: Typically 4–8 J/cm² per window. Do not stack all dosing on the anterior window; distribute across planes.
- Robot vs handpiece: Robot to cover broader capsular and periarticular fields; handpiece for focal medial joint line tenderness, pes anserine bursitis, or patellar tendon nodules.
- Schedule: Chronic OA—12 sessions; reassess after 6. Reinforce gait training, quadriceps/hip abductor strengthening, and weight management.
- Rationale: Distributed dosing respects joint geometry and reflective surfaces. Posterior access often improves results by reaching synovium/capsule and posterior neurovascular inflow, augmenting microcirculatory and anti-nociceptive effects.
Plantar Fasciitis and Foot-Pain Syndromes: Corridor Thinking
- Position: Prone or seated with ankle neutral to slight dorsiflexion.
- Targeting: Medial calcaneal tubercle, proximal fascia, abductor hallucis, and flexor retinacula corridors; consider tibial nerve and branches (Baxter’s nerve) if neurogenic components are suspected.
- Energy density: 4–8 J/cm²; robot across a defined plantar field; handpiece for focal trigger points and nerve entrapment corridors.
- Schedule: Often 6–12 sessions depending on chronicity; combine with calf flexibility work, intrinsic foot strengthening, footwear/orthoses as indicated.
- Rationale: Treat the fascia, but do not forget proximal and distal kinetic links—calf complex stiffness, tibial nerve mechanics, and midfoot locking patterns.
Peripheral Neuropathic Pain and Nerve Irritability
- Corridor approach: Follow the nerve’s path from distal to proximal, addressing known entrapment sites (e.g., tarsal tunnel, fibular neck) and segmental paraspinal contributors to radicular pain.
- Energy density: 4–8 J/cm²; titrate based on sensitivity. Favor a non-contact robot over highly allodynic skin; use the handpiece gently if tolerated.
- Schedule: 12 sessions are common for chronic neuropathic states; measure gains via pain descriptors (burning/electric), vibration thresholds, monofilament mapping, and sleep quality.
- Rationale: MLS laser can modulate nociceptor activity, microcirculation, mitochondrial function in Schwann cells and axons, and neuroimmune crosstalk, contributing to symptom relief and functional recovery.
Post-Surgical Scenarios: Non-Contact Advantages
- Indications: Scar modulation, edema reduction, pain control, and range-of-motion restoration.
- Technique: Robotic non-contact dosing preserves sterility and comfort. Avoid direct pressure on sensitive tissues.
- Energy density: Typically 4–6 J/cm² early; expand to 6–8 J/cm² as tolerated and per healing stage.
- Schedule: 6–12 sessions over 2–4 weeks; coordinate with physical therapy timelines.
- Rationale: Early photobiomodulation can ease pain, support microcirculation, and promote organized collagen remodeling while minimizing tactile provocation.
Fracture Healing Considerations: Timing and Scope
A pragmatic note from clinical experience: while fracture photobiomodulation is often referenced as off-label depending on jurisdiction and device labeling, I have observed compelling clinical responses when initiated within the first 7–10 days after injury in appropriate cases. Targeting the fracture zone and periosteal envelope with carefully titrated densities may support the inflammatory and early reparative phases. For established nonunions, results are mixed; I typically reserve laser in this context as an adjunct to an overall program (e.g., orthobiologic strategies, stabilization). Always coordinate with the treating orthopedist and adhere to local regulatory guidance.
Orthobiologics Integration: Pre-, Day-Of-, and Post-Injection Protocol Logic
Regenerative outcomes depend on biological processes that unfold over weeks. MLS laser can amplify constructive signals without blunting the essential early inflammatory phase of PRP or related orthobiologics when parameters and timing are selected intelligently.
- Pre-injection priming (2–3 sessions): “Prep the soil.” Focus on microcirculation, lymphatic readiness, and nociceptive downshift to normalize tone and improve local homeostasis. Typical densities: 4–6 J/cm² over the target region and relevant kinetic chain contributors.
- Day of injection: Use a program aligned to supportive vasomodulation and comfort without imposing heavy anti-inflammatory signatures. Non-contact robotic dosing can be ideal to avoid tactile provocation.
- Post-injection series (?6 sessions): Space at 24–48 hour intervals in the first two weeks, then taper. Maintain densities within 4–8 J/cm², adjusting to tolerance. The aim is to reduce excessive pain, improve microcirculation, and facilitate cellular bioenergetics that underwrite remodeling.
Preliminary and evolving data suggest that photobiomodulation can enhance PRP outcomes, with some clinics observing clinically meaningful additive benefits. In my practice, patients receiving MLS in a structured peri-injection protocol often report faster comfort recovery and earlier rehab engagement.
Mechanistic Cascade: From Rapid Analgesia to Mitochondrial Remodeling
Understanding the “why” behind the therapy helps us dose wisely and counsel accurately.
- Early analgesia (hours):
-
- Modulation of nociceptor channel activity (e.g., TRPV1 and related ion channels).
- Gate-control effects at the spinal segmental level as peripheral input normalizes.
- Improved microvascular flow reduces ischemic metabolites and peripheral sensitization.
- Subacute neuroimmune recalibration (days):
-
- Reduced pro-inflammatory cytokine signaling (e.g., TNF-?, IL-1?) and support of pro-resolving pathways.
- Lymphatic mobilization decreases local edema, improving tissue oxygenation.
- Normalization of glial reactivity in peripheral and potentially central circuits helps reduce hyperalgesia and allodynia.
- Mitochondrial photobiology (days to weeks):
-
- 808 nm light interacts with chromophores, including cytochrome c oxidase, enhancing electron transport and ATP production.
- Controlled ROS signaling acts as a second messenger, upregulating antioxidant defenses and pro-repair gene expression.
- Improved mitochondrial density and function (with adequate nutrition, sleep, and mechanical load) underwrite connective tissue remodeling and the endurance of pain relief.
Pulse-structured 905 nm contributes to deeper penetration and synchronized on–off energy delivery, preserving thermal neutrality while maintaining signaling efficiency.
Avoiding Bioinhibition: Distribute Dose, Don’t Stack
When a patient asks for “more,” resist the temptation to extend time on the same field beyond your density target. Instead:
- Add posterior or medial windows for joints.
- Treat the contralateral or proximal kinetic contributors (e.g., hip abductors in knee OA).
- Use the handpiece to clear trigger points that perpetuate nociception upstream or downstream.
This respects the Arndt–Schulz curve and often yields better clinical responses than overconcentrating the dose in a single window.
Sensation, Safety, and Reassurance
Patients often ask, “Should I feel heat?” With MLS dual-wavelength, short-pulse architecture, the answer is usually no. If a patient is very sensitive and feels slight warmth or tingling, I reassure them that it is common and safe. I always verify comfort, skin integrity, and device settings. Educating patients about pulse cycles and energy absorption builds trust and reduces anxiety.
Device Reliability and Service
From a practical standpoint, robotic MLS systems have demonstrated durable performance in clinical use. The largest risk in my experience has been transport and installation, not daily operation. Robust field service networks that perform on-site repairs reduce shipping risks and downtime. Comprehensive on-site training at installation sets teams up for success.
Packages, Adherence, and Documentation
- Packaging: Frame care around 6 (acute) or 12 (chronic) sessions from the start. This aligns expectations and supports completion through the consolidation phase.
- Scheduling: Aim for 24 hours between early sessions when possible, or three sessions per week.
- Documentation: Track pain scales, function tests (sit-to-stand, walk tests), range of motion, and patient-reported outcomes. For neuropathic pain, include sensory mapping.
- Guidance: Encourage pacing of activity, hydration, and sleep—simple supports that leverage photobiomodulation’s physiological benefits.
Combining with Shockwave, Exercise, and Mitochondrial Supports
- Shockwave (ESWT): I often pair laser and ESWT in chronic tendinopathies. ESWT may be used to “mechanically signal” the tendon mid-substance; MLS sessions in the surrounding days can modulate pain and support microcirculation and mitochondrial capacity. Sequence and spacing are individualized.
- Exercise therapy: Progressive loading is essential to convert laser-driven comfort into tissue resilience. I coordinate MLS sessions around key rehab days to reduce pain and facilitate proper motor patterning.
- Nutritional and mitochondrial supports: While specific supplementation is a provider–patient decision, principles include adequate protein, micronutrients, omega-3s as appropriate, and consideration of mitochondrial cofactors (e.g., CoQ10) where clinically indicated. Avoid blanket anti-inflammatory suppression in early regenerative windows unless medically necessary.
Practical Q&A-Inspired Pearls
- Why distribute the dose around a joint? Because geometry and reflectivity (e.g., patella) limit anterior-only dosing. Posterior and medial windows access capsular and synovial targets more effectively.
- Can lasers replace surgery? It can reduce pain and sometimes delay surgery by improving function and calming inflammation, but it will not reverse end-stage structural issues (e.g., true bone-on-bone). Be transparent.
- What if the patient feels nothing after session 1? Normal. Ask them to test the function at 4–6 hours and again after session 3. Set expectations around cumulative effects.
- How do I titrate density? Start in the 4–6 J/cm² range for acute and sensitive presentations; move toward 6–8 J/cm² for chronic, tolerant tissues. Respect the patient’s feedback and observable responses.
- Is there a “best” window for PRP? Pre-injection priming (2–3 sessions), day-of gentle support, and 6 post-injection sessions is a prudent and commonly used pattern. Calibrate settings to support, not suppress, intended inflammatory phases.
Exploring Integrative Medicine- Video
Extended Physiological Deep Dive: Chromophores, Redox, and Tissue Remodeling
- Chromophore interactions: 808 nm photons interact with cytochrome c oxidase, modulating electron transport. Bound nitric oxide can be photodissociated, freeing the enzyme and enhancing oxygen utilization. Hemoproteins and photoacceptors in vascular endothelium also respond, supporting vasodilation.
- Redox signaling: Low-level increases in ROS serve as signaling cues—inducing Nrf2 pathways, improving antioxidant defenses, and tuning inflammatory gene expression. Photobiomodulation’s power lies in its ability to use sub-toxic signals to guide cells toward homeostasis.
- Connective tissue remodeling: Fibroblasts and tenocytes can shift from a catabolic/inflamed phenotype toward balanced matrix production under improved energy and oxygenation. Collagen fibrillogenesis and cross-link maturation occur over weeks; hence, the importance of completing 6–12 sessions and integrating progressive mechanical loading.
- Neural effects: Peripheral nociceptor excitability can drop; conduction in small myelinated fibers may normalize; neuroimmune glial activity can downshift pro-inflammatory signaling. Central sensitization may ease as peripheral input calms.
- Vascular and lymphatic effects: Angio-supportive signaling and improved lymphatic pumping reduce edema, enhance oxygen delivery, and clear metabolites—critical for tendon insertions, plantar fascia, and arthritic joints.
Contraindications, Precautions, and Scope
- General cautions: Avoid direct eye exposure; use protective eyewear. Be cautious over known malignancies, active hemorrhage, or the gravid uterus without clear indication and interprofessional guidance. Respect device labeling and local regulations.
- Post-PRP: Align parameters to support regenerative intent; avoid aggressive anti-inflammatory measures unless medically necessary.
- Fractures: As noted, consider regulatory guidance; coordinate with orthopedics.
A Clinician’s Workflow Summary
- Intake and assessment: Define pain generators and contributing factors. Establish function metrics.
- Patient setup: Prioritize comfort and stillness; choose a contact vs. a non-contact approach.
- Field definition: Zero X–Y; center epicenter; expand to include connective-tissue corridors.
- Dose: Select energy density (4–10 J/cm²) by condition and acuity. Let the software auto-calculate the time for the field size.
- Hybridization: Robot for fields; handpiece for focal trigger points and dynamic testing as appropriate.
- Scheduling: Acute 6 sessions; chronic 12; M–W–F cadence. Educate about cumulative effects.
- Integration: Coordinate with PT, ESWT, orthobiologics; plan pre/day-of/post timing when relevant.
- Reassessment: Review pain, function, and tolerance at sessions 3–5 and at completion. Adjust windows and densities as responses dictate.
Clinical Observations in Context
From my experience, the best outcomes emerge when the MLS laser is embedded inside a broader plan:
- For low back with facet pain: Add core stabilization, hip-hinge training, and gluteal activation during or shortly after the series, as pain permits.
- For knee OA: Combine with quadriceps/hip strengthening, gait retraining, and weight optimization.
- For plantar fasciitis: Address calf flexibility, foot intrinsic strength, and footwear.
- For neuropathic pain: Layer in graded desensitization and nerve glide strategies alongside sleep optimization.
Consistently, the patients who complete the protocol and integrate these behaviors sustain gains longer and defer invasive options more reliably.
References
- World Association for Laser Therapy (WALT) recommendations on laser phototherapy dosing (J/cm²) and condition-specific guidance.
- Hamblin MR. Mechanisms and applications of photobiomodulation. Photochem Photobiol Sci. Multiple publications.
- Anders JJ, Lanzafame RJ, Arany PR. Photobiomodulation: underlying mechanisms and cellular pathways. Seminars in Cutaneous Medicine and Surgery.
- Chung H et al. The nuts and bolts of low-level laser (light) therapy. Ann Biomed Eng.
- Chow RT et al. Efficacy of low-level laser therapy in neck pain: a systematic review and meta-analysis. Lancet.
- WALT dosage tables and consensus statements across musculoskeletal indications.
- Clinical device manuals and software dosing logic for MLS dual-wavelength systems (manufacturer documentation).
- Emerging studies on laser plus orthobiologics (PRP) synergy in musculoskeletal care.
Note: Some indications and integration protocols are evolving as research progresses; consult current guidelines and device labeling.
Keywords
MLS laser therapy, photobiomodulation, 808 nm, 905 nm, energy density, J/cm², Arndt–Schulz, bioinhibition, facet syndrome, low back pain, knee osteoarthritis, plantar fasciitis, peripheral neuropathy, post-surgical recovery, orthobiologics, PRP, mitochondrial biogenesis, microcirculation, nociception, neuroimmune modulation, connective tissue remodeling, shockwave integration, rehabilitation, dosing protocols, robotic laser, handpiece, collimation, X–Y field.
Summary
The core message remains: modern MLS laser therapy should be delivered as energy-density–based care, not raw joules, with precise targeting and patient-centered setup. I prioritize comfort and stillness, align the robotic head with a defined X–Y field, and add a handheld diode for focal trigger points. I distribute doses across relevant anatomic windows—anterior, medial, and posterior for knees; paraspinal and fascial corridors for low backs—rather than stacking energy in one place. The software’s automatic calculation of time-to-area changes helps maintain dosing fidelity.
Physiologically, patients may feel improved comfort at 4–6 hours due to nociceptive and microvascular shifts. By sessions 3–5, we often see functional improvements as neuroimmune and hemodynamic benefits consolidate. By sessions 6–12, mitochondrial and connective tissue remodeling support more durable gains. For acute cases, six sessions are a practical minimum; for chronic conditions, twelve sessions typically provide a robust foundation. Packaging care helps patients finish the plan.
With orthobiologics, I use a 2–3-session pre-injection priming, a day-of supportive session, and 6 sessions post-injection to enhance integration without blunting the intended early inflammatory phase. MLS lasers’ non-thermal, dual-wavelength, short-pulse architecture enables high-peak-photon delivery while maintaining stable surface temperature. I encourage pairing laser with progressive exercise, selective shockwave, and lifestyle-based mitochondrial supports to convert analgesia into lasting function.
Conclusion
MLS laser therapy, when executed with methodical, evidence-aligned dosing and precise targeting, is a powerful adjunct for spine, joint, and soft-tissue conditions. The keys are:
- Dose to energy density (J/cm²), not total joules.
- Map treatment fields to the source and its connective corridors.
- Leverage pulse-structured dual wavelengths to deliver energy without heat buildup.
- Respect cumulative timelines: early analgesia, subacute neuroimmune shifts, and longer-horizon mitochondrial and matrix remodeling.
- Integrate with rehab and, when used, orthobiologics via pre-, day-of-, and post-protocols that “prep the soil” and support regenerative intent.
These principles—combined with patient-centered setup and clear expectations—consistently translate into improved comfort, function, and quality of life in my practice.
Key Insights
- Energy density governs outcomes; 4–10 J/cm² is a common therapeutic window.
- Robotic X–Y field control with automatic time recalculation improves dosing accuracy.
- Dual-wavelength MLS (808/905 nm) delivers high-peak, short-pulse energy with minimal surface heat, enhancing comfort and safety.
- Distribute the dose across anatomical windows to avoid bioinhibition and effectively reach synovial and capsular targets.
- Schedule for biology: 6 sessions for acute, 12 for chronic, with 24-hour spacing, early when possible.
- Pre-, day-of-, and post-PRP laser sessions can augment microcirculation and cellular energetics without suppressing beneficial inflammation.
- Combine with exercise therapy, shockwave when indicated, and supportive lifestyle/mitochondrial measures to convert analgesia into durable resilience.
Disclaimer: This educational content is provided by Dr. Alexander Jimenez, DC, FNP-APRN, for informational purposes only and does not constitute medical advice. It is not a substitute for individualized evaluation, diagnosis, or treatment. All individuals must obtain recommendations for their personal situations from their own qualified medical providers.
General Disclaimer
Professional Scope of Practice *
The information herein on "Benefits of Therapeutic Approaches for Tissue Regeneration" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics