Table of Contents
Introduction
When issues like autoimmune disorders start to affect the body for no reason, it can lead to chronic problems and conditions that can affect the various muscles and vital organs that cause overlapping risk profiles to the host. The body is a complex machine that allows the immune system to release inflammatory cytokines to the affected area when a person has acute or chronic pain. So when a person has an autoimmune disorder like fibromyalgia, it can affect their quality of life while amplifying painful sensations in their musculoskeletal system. Today’s article focuses on fibromyalgia and its systems, how this autoimmune disorder correlates with myofascial pain syndrome, and how chiropractic care can help reduce fibromyalgia symptoms. We refer our patients to certified providers that incorporate techniques and various therapies for many individuals with fibromyalgia and its correlating symptoms, like myofascial pain syndrome. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a fantastic way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer
What Is Fibromyalgia?
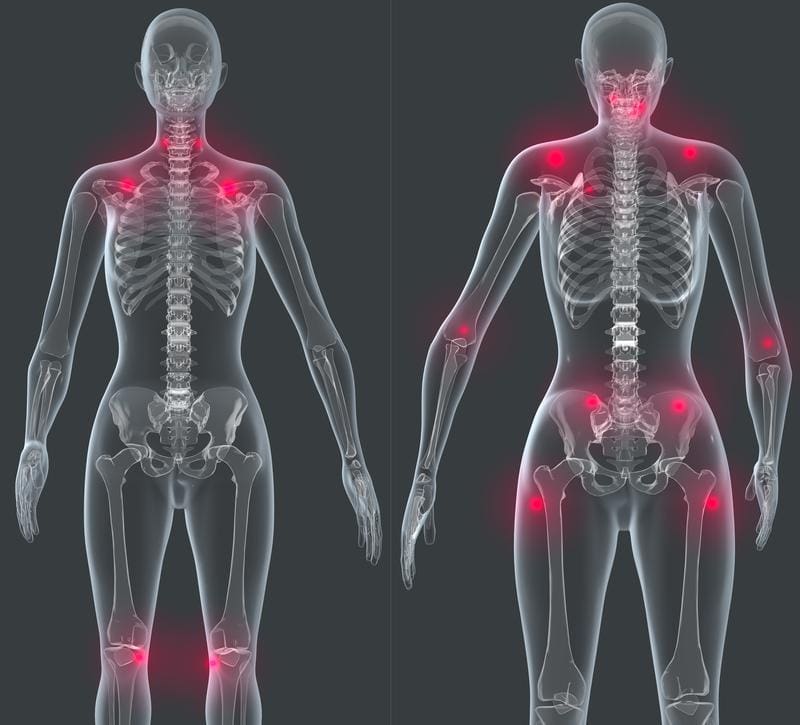
Have you been dealing with unquestionable pain that is affecting your daily life? Do you feel fatigued when you are barely getting out of bed? Or have you been dealing with brain fog and aches all over your body? Many of these symptoms overlap with an autoimmune disorder known as fibromyalgia. Studies reveal that fibromyalgia is an autoimmune condition characterized by widespread chronic musculoskeletal pain that can correlate with neurosensory disorders that affect the nervous system. Fibromyalgia can affect about 4 million adults in America and roughly 2% of the general adult population. When people with fibromyalgia go through a physical examination, the test results would appear to be normal. That is because fibromyalgia can include multiple tender points in specific body areas and manifest as a primary or secondary condition while extending far beyond the defining criteria. Additional studies reveal that the pathogenesis of fibromyalgia could potently be linked with other chronic factors that affect the following systems:
- Inflammatory
- Immune
- Endocrine
- Neurological
- Intestinal
The Symptoms
Many individuals, especially women, have fibromyalgia, which causes symptoms of multiple somato-visceral issues. To that point, it can often overlap and accompany fibromyalgia. Unfortunately, fibromyalgia is challenging to diagnose since the pain can last for several months to years. Studies have shown that even though fibromyalgia is challenging to diagnose when many other factors like genetics, immunological, and hormonal factors potentially play a part in this autoimmune disorder. Also, additional symptoms and specific diseases like diabetes, lupus, rheumatic diseases, and musculoskeletal disorder can be associated with fibromyalgia. Some of the following symptoms that many fibromyalgia individuals deal with include:
- Fatigue
- Muscle Stiffness
- Chronic Sleep Issues
- Trigger Points
- Numbness and Tingling sensation
- Abnormal menstrual cramps
- Urinary issues
- Cognitive issues (Brain Fog, Memory loss, Concentration issues)
An Overview Of Fibromyalgia-Video
Have you been having trouble getting a good night’s sleep? Do you feel pain in different areas of your body? Or have you been dealing with cognitive issues like brain fog? Many of these symptoms correlate with an autoimmune disorder known as fibromyalgia. Fibromyalgia is an autoimmune disorder that is challenging to diagnose and can cause immense pain to the body. The video above explains how to notice the signs and symptoms of fibromyalgia and what associated conditions correlate with this autoimmune disorder. Since fibromyalgia causes widespread musculoskeletal pain, it can even affect the peripheral and central nervous systems. This causes the brain to send out neuron signals to cause an increase in sensitivity to the brain and spinal cord, which then overlaps with the musculoskeletal system. Since fibromyalgia causes pain to the body, it can present unrecognized symptoms that can be difficult to recognize and can be arthritis-related.
How Fibromyalgia Is Correlated With Myofascial Pain Syndrome
Since fibromyalgia can correlate with different chronic conditions, one of the most chronic disorders can mask the effects of fibromyalgia in the body: myofascial pain syndrome. Myofascial pain syndrome, according to Dr. Travell, M.D.’s book, “Myofascial Pain Syndrome and Dysfunction,” mentions that when a person has fibromyalgia causes musculoskeletal pain, overtime if not treated, can develop trigger points in the affected muscles. This causes muscle stiffness and tenderness in the taut muscle band. Additional studies mentioned that since myofascial pain syndrome and fibromyalgia have common muscular pain symptoms, they can cause tenderness and refer pain to different body locations. Fortunately, available treatments can help reduce the muscular pain symptoms caused by fibromyalgia associated with myofascial pain syndrome.
Chiropractic Care & Fibromyalgia Associated With Myofascial Pain
One of the available treatments that can help relieve the muscular pain from fibromyalgia associated with myofascial pain syndrome is chiropractic therapy. Chiropractic therapy is a safe, non-invasive treatment option that can help alleviate symptoms of body pain and swelling from a spinal subluxation. Chiropractic care uses manual and mechanical manipulation to re-align the spine and improve nerve circulation while increasing blood flow back to the joints and muscles. Once the body has been re-balanced from chiropractic therapy, the body can manage symptoms better and reduce the effects of fibromyalgia. Chiropractic therapy also provides a customized treatment plan and works with associated medical professionals to achieve maximum results and ensure the highest quality of life for the individual.
Conclusion
Fibromyalgia is one of the most common autoimmune disorders that affect most of the population and can be challenging to diagnose. Fibromyalgia is characterized by widespread chronic musculoskeletal pain that can correlate with neurosensory disorders and cause pain symptoms in the body. People with fibromyalgia also deal with myofascial pain syndrome, as both disorders cause muscle and joint pain. Luckily, treatments like chiropractic therapy allow spinal manipulation of the body to be re-aligned and restore functionality to the host. This reduces the symptoms caused by fibromyalgia and causes the individual to be pain-free and function normally.
References
Bellato, Enrico, et al. “Fibromyalgia Syndrome: Etiology, Pathogenesis, Diagnosis, and Treatment.” Pain Research and Treatment, U.S. National Library of Medicine, 2012, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3503476/.
Bhargava, Juhi, and John A Hurley. “Fibromyalgia – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 10 Oct. 2022, https://www.ncbi.nlm.nih.gov/books/NBK540974/.
Gerwin, R D. “Myofascial Pain and Fibromyalgia: Diagnosis and Treatment.” Journal of Back and Musculoskeletal Rehabilitation, U.S. National Library of Medicine, 1 Jan. 1998, https://pubmed.ncbi.nlm.nih.gov/24572598/.
Simons, D. G., and L. S. Simons. Myofascial Pain and Dysfunction: The Trigger Point Manual: Vol. 2:the Lower Extremities. Williams & Wilkins, 1999.
Siracusa, Rosalba, et al. “Fibromyalgia: Pathogenesis, Mechanisms, Diagnosis and Treatment Options Update.” International Journal of Molecular Sciences, U.S. National Library of Medicine, 9 Apr. 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8068842/.
Disclaimer
General Disclaimer
Professional Scope of Practice *
The information herein on "Myofascial Pain Syndrome Associated With Fibromyalgia" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics