Table of Contents
Introduction
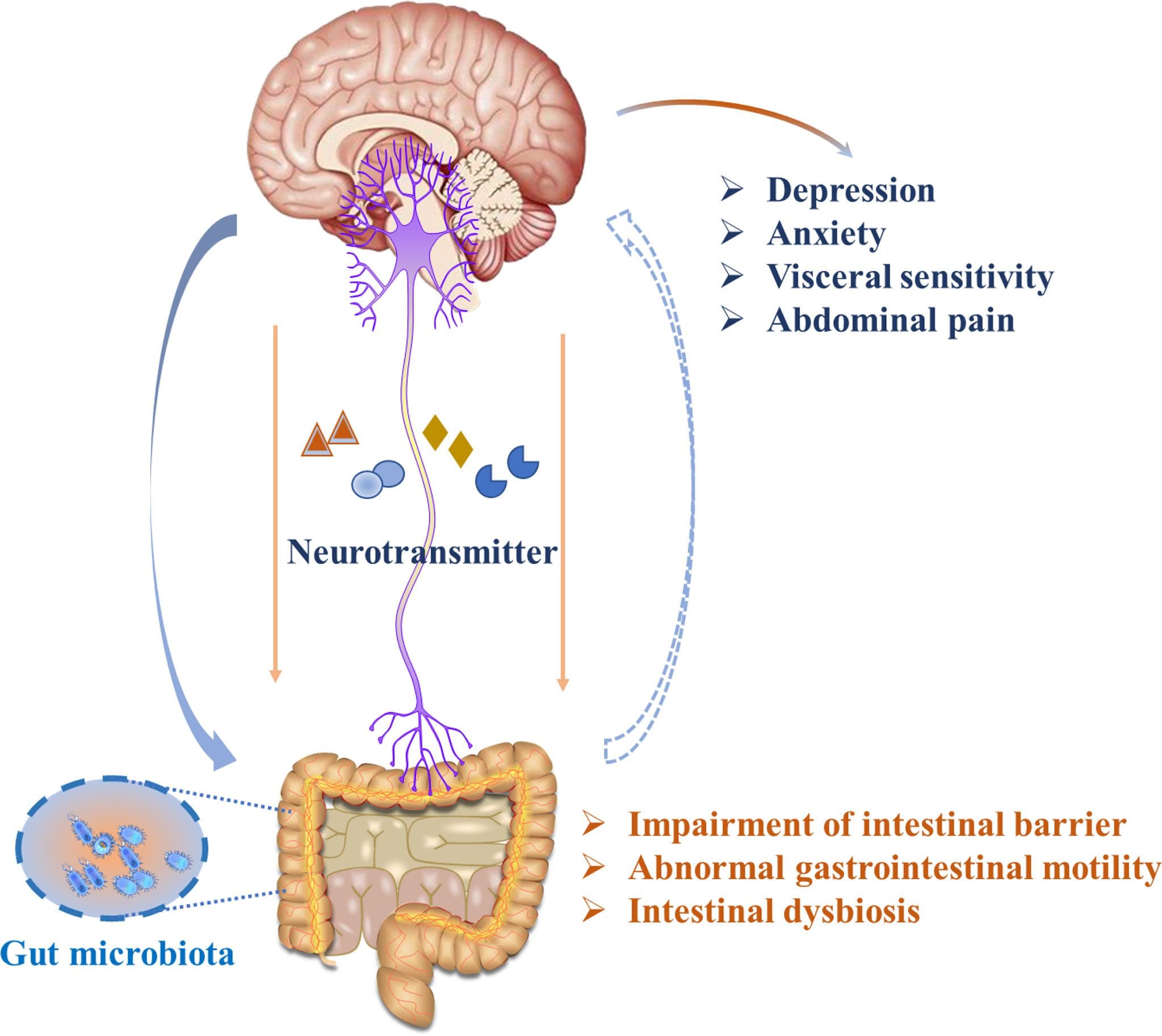
The gut-brain axis is fundamental to the body as it communicates bi-directional with the brain and the gut. Separately they provide different functions that are required of the body. The brain, part of the central nervous system, allows the neurons to travel to each overlapping nerve root while having a causal relationship with different muscles and organs connected to the spinal cord. While the gut, which is part of the gastrointestinal and digestive system, helps modulate the body’s homeostasis and regulates the immune system. The nerves, muscles, and organs correspond as the nerve pathways interconnect to the spinal cord. When injuries or traumatic events affect the body, it can lead the individual to suffer from pain affecting their body while increasing the risk associated within different locations. For example, chronic stress causing gut inflammation is associated with headaches or neck and back pain. Today’s article focuses on the gut-brain axis, what happens when chronic issues affect the gut-brain axis, and how somatovisceral pain affects the gut-brain axis. We refer patients to certified providers specializing in gastroenterology treatments that help those with issues that affect the gut-brain axis and overlapping problems impacting the body. We also guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is the solution to asking our providers insightful questions. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
How Does The Gut & Brain Work Together?
The way the gut and brain correlate together is quite remarkable. The gut allows food to be digested in the stomach to be bio-transformed into nutrients the body needs to function. While the brain sends neuron signals through the spinal cord, those signals help provide the sensory-motor functions to make the body move. Now, how do the brain and gut work together in the body? Well, studies reveal that the gut-brain axis correlates to the various systems like the autonomic nervous system, the HPA axis, and the nerves surrounding the gastrointestinal tract help the brain influence intestinal activity and regulate cognitive function. Each of these vital organs has a causal relationship where they:
- Help with sleep regulation
- Improve memory functionality
- Helps coordinate physical and emotional well-being
- Regulating inflammatory responses
When chronic issues affect the gut-brain axis, it can cause an overlap in risk profiles that rise in the body and not just in the brain or the gut. Studies reveal that issues that begin to affect the gut-brain axis can cause alteration within the bi-directional pathway and trigger other problems that correlate to the body.
Chronic Issues Affecting The Gut-Brain Axis
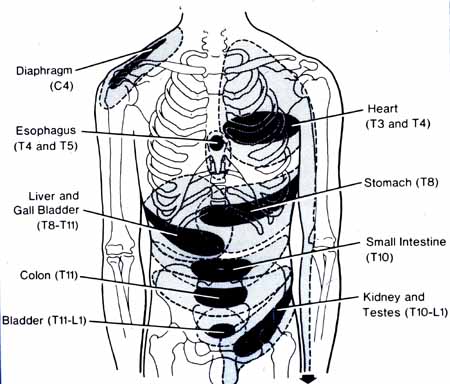
Have you been suffering from fatigue? How about reoccurring headaches that never seem to go away? Do digestive complaints like IBS, GERD, or gut inflammation affect more than your gut? These chronic issues can be various factors that impact the bi-directional connection of the gut-brain axis. Stress, gut inflammation, traumatic events, food allergens, autoimmunity, and metainflammation are some overlapping risk profiles associated with neck and back pain. Studies reveal that chronic stress in the brain can affect the gut’s composition and functionality by alternating intestinal permeability. When the gut microbiome is being affected, the harmful bacteria begin to overproduce and trigger the sympathetic branch of the nervous system to cause an imbalance of hormones to be released and be associated with stress-related muscle dysfunction in the body. So what does this implicates to the body? Let’s say, for example, that you have been experiencing pain in the cervical region of the spine, but your brain is telling the body that it is a headache. This is known as somato-visceral pain.
An Overview Of Somatosensory Tract-Video
Have you been suffering from cognitive and memory dysfunction? How about experiencing gastrointestinal issues that are affecting your gut? Or have you experienced any cramping, gnawing, or sharp pain that seems to be triggered by movement and appears in one area of the body? This is known as somato-visceral pain and is defined as soft tissues and muscles experiencing pain that can affect the internal organs. Somato-visceral pain is much easier to identify than viscero-somatic pain because visceral pain is caused by damaged internal organs associated with distress in different body locations. At the same time, somato-visceral pain is often associated with musculoskeletal pain. The video above explains the somatosensory tract that is in the body and how the body responds to the somatosensory system. The somatosensory system is located within the peripheral and central nervous systems. It is responsible for modulating the body’s sense of touch, vibration, temperature, and pain receptors that are located in the body. When traumatic events affect the somatic nerves, they can trigger changes in the gut-brain axis and cause alterations to the affected organs.
Somatovisceral Pain Affecting The Gut-Brain Axis
When dealing with chronic stress, the effects cause a dysfunctional gut-brain axis and cause issues affecting the two organs. Studies reveal that when chronic stress becomes an associated mediator for gut disturbances and dysregulation of the gut-brain axis, it can cause an overlap in risk profiles in the body. So what does this mean, and how is the body affected by somato-visceral pain? First, let’s look at what happens when the body is affected by chronic stress. When stress affects the gut and the brain, it can cause issues like IBS (irritable bowel syndrome) or headaches. Studies reveal that IBS is one of the most common gastrointestinal disorders that trigger visceral and somatic hypersensitivity on the sensory nerves. So the body experiencing sharp pain in the back or neck may be associated with IBS.
Now looking at headaches and their causes on the body, it is one example of somato-visceral pain. When a person is dealing with neck trauma due to an auto accident that causes whiplash can trigger cervicogenic headache. How do the two correlate with somato-visceral pain? Well, somato-visceral pain is when soft muscles and tissues are affected and can cause an impact on the internal organs. For cervicogenic headaches may trigger mechanical pain along the cervical spine to be aggravated by movement and be associated with musculoskeletal issues like rheumatoid arthritis, ankylosing spondylitis, or muscle strain on the upper cervical spine. Many individuals go to available treatments that can help them better understand the issue that is causing them to be in pain and how to alleviate them.
Conclusion
The gut-brain axis is fundamental in the body as it communicates bi-directional with the brain and the gut. These two organs help keep the body functioning as the brain provides neuron signals while the gut regulates homeostasis. The gut-brain axis helps the body by correlating with the various systems that help influence intestinal activity and control cognitive function. When traumatic factors affect the body’s soft tissues and muscles and trigger organ issues, this is known as somato-visceral pain. Somato-visceral pain is when the muscles are affecting the organs, and an example is cervical muscle strain associated with headaches. Providing much-needed information on available treatments can help many individuals when being examined by their physicians.
References
Appleton, Jeremy. “The Gut-Brain Axis: Influence of Microbiota on Mood and Mental Health.” Integrative Medicine (Encinitas, Calif.), InnoVision Health Media Inc., Aug. 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6469458/.
Carabotti, Marilia, et al. “The Gut-Brain Axis: Interactions between Enteric Microbiota, Central and Enteric Nervous Systems.” Annals of Gastroenterology, Hellenic Society of Gastroenterology, 2015, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4367209/.
Martin, Clair R, et al. “The Brain-Gut-Microbiome Axis.” Cellular and Molecular Gastroenterology and Hepatology, Elsevier, 12 Apr. 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6047317/.
Suslov, Andrey V, et al. “The Neuroimmune Role of Intestinal Microbiota in the Pathogenesis of Cardiovascular Disease.” Journal of Clinical Medicine, MDPI, 6 May 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8124579/.
Yuan, Yao-Zong, et al. “Functional Brain Imaging in Irritable Bowel Syndrome with Rectal Balloon-Distention by Using Fmri.” World Journal of Gastroenterology, Baishideng Publishing Group Inc, June 2003, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4611816/.
Disclaimer
General Disclaimer
Professional Scope of Practice *
The information herein on "The Gut-Brain Axis Affected By Somatovisceral Pain" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics