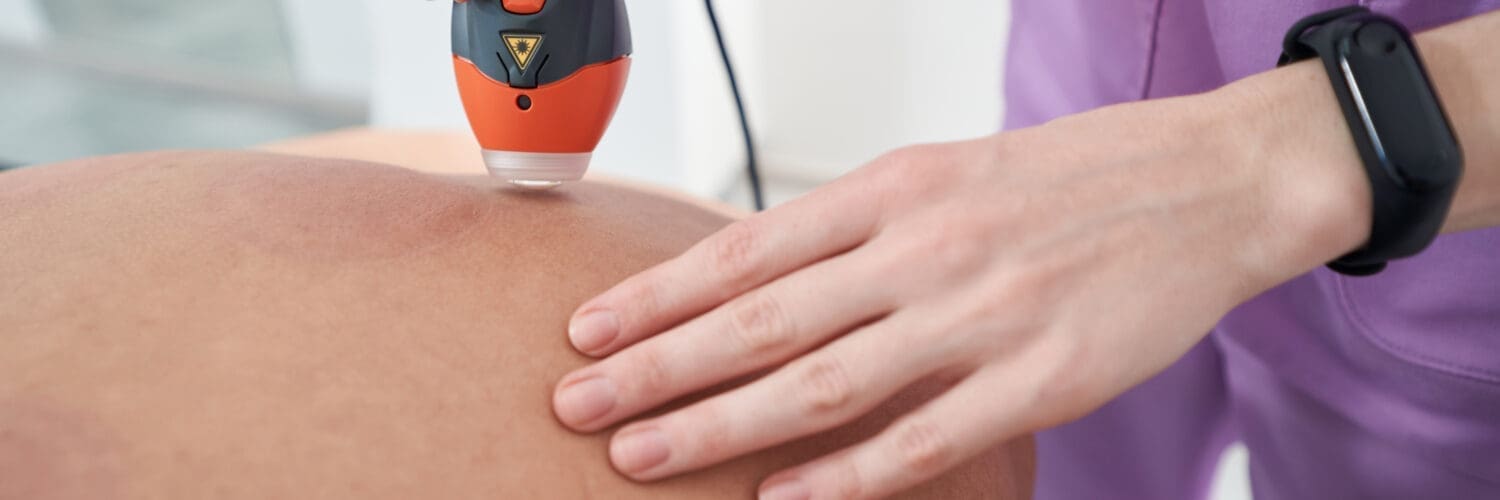
Uncover the science behind MLS laser therapy combined with photobiomodulation for effective treatment and recovery to the body.
Table of Contents
Introduction Abstract
As a clinician-scientist and integrative practitioner, I have long pursued therapies that meaningfully shift patient outcomes by improving cellular health, reducing pain, restoring functional capacity, and accelerating tissue repair. Over the last 10–15 years, the field of regenerative medicine has rapidly matured—transitioning from siloed practices into synergistic, cross-disciplinary care where orthobiologics (e.g., PRP, BMAC), shockwave modalities, and photobiomodulation (PBM) now work together to optimize mitochondrial function, modulate inflammation, and recalibrate neurovascular dynamics across complex musculoskeletal and neuropathic conditions. In this educational post, I present a comprehensive, evidence-based discussion of modern laser therapy—specifically MLS Robotic Laser Therapy—and its physiologic underpinnings, technical attributes, clinical applications, and validated outcomes. I will clarify terminology (laser therapy, photobiomodulation, “cold” versus “hot” lasers), address safety and dosing considerations, and explain why MLS’s multiwave locked system architecture (synchronized 808 nm continuous + 905 nm pulsed) produces class IV-level efficacy while maintaining a class III-like safety profile, minimizing thermal risk and maximizing cellular absorption via higher peak photon density without harmful heat accumulation.
Drawing on leading research and clinical registry data, we will examine how PBM interfaces with mitochondrial complexes (notably cytochrome c oxidase), upregulates ATP synthesis, drives nitric oxide signaling, and orchestrates photochemical, photothermal, and photomechanical responses that culminate in reduced nociception, enhanced microcirculation, accelerated lymphatic clearance, and improved extracellular matrix remodeling. I will cover dose parameters (energy density, exposure time), emission modalities (continuous, pulsed, chopped), optical tissue interactions (reflection, transmission, scattering, absorption), and how these physics align with practical protocols. We will discuss point-by-point versus scanning techniques, robotic hands-free delivery for consistent dosing, and the importance of focal point control over joint windows, implants, and tattooed skin. We will review indications spanning acute and chronic tendinopathies, osteoarthritis, neuropathic pain, post-surgical recovery, non-healing wounds, burns, and athletic performance (including delayed-onset muscle soreness), and provide rationales for session frequency, progression (acute vs. chronic), and co-management with orthobiologics and shockwave.
Importantly, I will incorporate clinical observations from my practice and HealthVoice360 coverage to contextualize how PBM integrates into comprehensive care plans—dietary modulation of inflammation, sleep optimization, graded loading, fascial and joint mechanics, and autonomic balance—while highlighting workflow efficiency through robotic automation and standardized software-guided dosing. We will also explore the evolving aesthetic and neuropathy applications, including EU-cleared devices for neuropathic pain, and examine real-world outcomes via Data Biologics registry analyses—demonstrating faster pain reduction, improved functional metrics, higher patient satisfaction, and sustained benefits at 24 months when MLS is combined with orthobiologics.
By the end, you will understand precisely how and why MLS laser therapy is applied, what physiologic mechanisms it engages, and how to reason through protocol selection based on tissue targets, pathology phase, comorbidities, and patient goals. We will conclude with an extensive summary and key insights synthesizing these concepts into clinical decision-making frameworks. I aim to demystify laser therapy, ground it in rigorous physiology and modern research, and offer practical pathways to implement PBM safely and effectively across regenerative medicine, sports medicine, chiropractic, and advanced nursing practice settings.
Modern Photobiomodulation Terminology and Core Concepts: Clarifying the Landscape
- Defining Photobiomodulation (PBM)
-
- PBM refers to the therapeutic use of non-ionizing light (typically visible and near-infrared) to modulate biological processes. It is often called laser therapy, low-level laser (historically), cold laser (marketing), or high-intensity laser (for class IV devices). The critical point is that PBM seeks to trigger beneficial cellular responses without causing thermal tissue damage.
- PBM wavelengths commonly fall in the therapeutic window of 600–1200 nm, where absorption by melanin, hemoglobin, and water permits effective tissue penetration and meaningful photochemistry.
- Laser Optical Tissue Interactions
-
- Reflection: A fraction of incident light reflects off the skin surface; minimizing reflection improves dosing efficiency.
- Transmission: Some light passes through tissue layers toward deeper targets.
- Scattering: Photons scatter, distributing energy throughout tissues but reducing direct intensity at a target.
- Absorption: The desired endpoint—chromophores (e.g., cytochrome c oxidase, hemoglobin) absorb photons, initiating downstream biochemical effects.
- Key Laser Attributes
- Source: Diode lasers are common in therapeutic PBM; MLS uses high-quality diodes manufactured in Italy.
- Power and Classification:
-
- Class III: ?0.5 W, historically associated with “low-level”/”cold” lasers.
- Class IV: >0.5 W, “high power,” enabling shorter treatment times and deeper coverage but potentially higher thermal risk if not controlled.
- Emission Modality:
-
- Continuous: Laser is always on.
- Pulsed: Laser alternates on/off at high frequency; true pulsing allows thermal relaxation and limits heat accumulation.
- Chopped/Interrupted Continuous: Mechanical or electronic occlusion of a continuous source; heat can still accumulate because the source doesn’t truly turn off.
- Wavelength:
-
- Determines tissue penetration and chromophore engagement.
- MLS employs 808 nm (continuous) and 905 nm (pulsed)—synchronized to amplify biological effects with minimal thermal burden.
Physiologic Foundations of Photobiomodulation: Why Light Modulates Healing
- Photochemical Effects
-
- Cytochrome c Oxidase (CCO) Activation: Near-infrared photons absorbed by CCO enhance electron transport chain kinetics, increasing ATP synthesis and cellular energy availability. Increased ATP fuels reparative processes: protein synthesis, ion pump regulation, cytoskeletal remodeling.
- Nitric Oxide (NO) Modulation: PBM can transiently displace NO from mitochondrial complexes, improving respiration; additional NO promotes vasodilation, thereby augmenting perfusion and nutrient delivery.
- Reactive Oxygen Species (ROS) Signaling: Low-level ROS can act as signaling molecules, upregulating transcription factors (e.g., NF-?B, Nrf2) that regulate antioxidant defenses and repair cascades. PBM calibrates ROS below damaging thresholds, supporting adaptive responses.
- Photothermal Effects
-
- Gentle thermal elevation from PBM facilitates vasodilation, microcirculatory enhancement, and lymphatic drainage, aiding edema reduction and clearance of inflammatory mediators. Crucially, therapeutic PBM should remain below ~43°C to avoid inhibiting biological reactions and far below ~45°C to avoid thermal tissue damage.
- Photomechanical Effects
-
- Rapid nanosecond pulsing can cause micro-deformations in the extracellular matrix (ECM) and cell membranes, modulating mechanotransduction pathways that influence inflammation resolution, fibroblast activity, and collagen lattice organization. This mechanical signaling complements photochemical and photothermal responses, accelerating tissue repair.
- Neurophysiologic Pain Modulation
- PBM reduces nociceptor firing through:
-
-
- Downregulation of pro-inflammatory cytokines (e.g., IL-1?, TNF-?).
- Stabilization of neuronal membrane potentials and improved axonal transport.
- Enhanced endorphin and enkephalin dynamics in local tissue environments.
-
-
- PBM’s analgesia is non-opioid, non-NSAID, and achieved by modulating rather than suppressing inflammation—beneficial when paired with orthobiologics that depend on controlled inflammatory signaling for regenerative effects.
MLS Laser Therapy: Multiwave Locked System Architecture and Safety-Efficacy Balance
- What Is MLS?
-
- MLS (Multiwave Locked System) synchronizes 808 nm continuous emission with 905 nm pulsed emission, delivering energy simultaneously to superficial and deeper tissues while preventing continuous thermal build-up.
- The synchronized pattern produces homogeneous energy distribution—reducing “stone unturned” phenomena typical of unsynchronized multi-wavelength systems. Think of unsynchronized multi-wavelengths as a meteor shower with scattered coverage; MLS creates a coordinated energy “wavefront,” saturating target tissues evenly.
- Why MLS Achieves Class IV Efficacy with Class III-Like Safety
-
- High Peak Power, Low Mean Thermal Load: True pulsing at 905 nm enables elevated peak photon density—enhancing cellular absorption—while the off periods allow thermal relaxation and tissue cooling.
- Avoiding Thermal Thresholds: MLS delivery profiles remain below ~43°C in treated tissues, sidestepping the non-therapeutic window (43–45°C) and staying well below the threshold for thermal damage (>45°C), even during point-by-point dosing over focal targets.
- Wavelength Rationale
-
- 808 nm: Strong penetration, robust interaction with CCO; supports ATP upregulation and microvascular dynamics.
- 905 nm: Deep tissue reach with effective pulsed delivery; enhances photon density at depth for improved mitochondrial and ECM signaling while limiting heat.
- Emissive Modality Rationale
-
- Synchronized Emission: Maximizes combined benefits (photochemical + photomechanical) while controlling thermal effects, increasing the likelihood of biologically effective photon absorption by target tissues.
- Clinical Evidence and Adoption
-
- MLS has hundreds of publications and a global install base (~40,000 devices), with robust outcomes across MSK pain syndromes, post-op recovery, neuropathy, and wound care.
Laser Dosing Science: Parameters, Action Depth, and Practical Protocols
- Determinants of Action Depth
-
- Wavelength: Primary determinant; longer near-infrared wavelengths penetrate deeper.
- Emission Modality: Pulsed emission enables higher instantaneous peak power and photon density, increasing the chance of absorption at deeper targets without heat build-up
- Power Density (W/cm²): Higher power density at the focal spot improves dose delivery; MLS optics and focal control help concentrate energy where needed.
- Exposure Time: Governs total energy (Joules) delivered; dosing is titrated to pathology and target volume.
- Energy Units and Dosing
-
- Joules (J): Total energy delivered; J/cm² is energy density. Protocols adapt J/cm² based on tissue type, chronicity, and depth.
- Cumulative Treatments: PBM is cumulative—each session builds on prior mitochondrial and vascular adaptations. Acute cases often need 4–6 sessions; chronic cases 8–12 or more, delivered 2–3 times per week, depending on access and clinical urgency.
- Thermal Safety
-
- A core MLS advantage is the ability to perform point-by-point dosing safely (with a class III-like thermal profile), enabling precision along joint lines, tendon insertions, or wound margins without risking thermal injury.
Technique Optimization: Point-by-Point versus Scanning, Robotics, and Focal Control
- Point-by-Point Delivery
-
- Ideal for focal lesions (e.g., tendon entheses, joint spaces, neuromas). Provides precise dosing at target sites. MLS’s pulsed profile prevents heat accumulation even during stationary application.
- Scanning Delivery
-
- Useful for diffuse pathology (e.g., large fascial pain fields). Operator-dependent uniformity is a challenge; robotic systems solve this by standardizing scan patterns and dose uniformity.
- Robotic Hands-Free Systems (e.g., MLS M7)
-
- Consistency: Automated dosing ensures identical energy delivery across sessions and operators, improving reproducibility and outcomes.
- Workflow Efficiency: Staff can set up and supervise treatment while performing concurrent tasks (e.g., shockwave on a different region or manual therapy). Hands-free delivery also allows simultaneous adjunctive maneuvers (trigger point release, positional biasing).
- Software-Driven Dosing: Anatomically guided interfaces generate therapeutic dose recommendations based on body region, pathology phase, and patient characteristics, ensuring proper J/cm² without operator guesswork.
- Focal Point and Windowing
-
- Bone reflects >90% of incident class IV laser energy—strategically position optics to deliver through joint windows or soft tissue corridors to reach target tissues (e.g., intra-articular synovium, ligament attachments).
- Implants and Tattoos: MLS can be used safely over surgical implants and tattooed skin due to its lower thermal profile and controlled emission pattern—an uncommon capability among class IV lasers.
Clinical Mechanisms and Outcomes: From Inflammation Modulation to Tissue Repair
- Inflammation Modulation (Not Suppression)
-
- PBM shifts the inflammatory milieu by upregulating anti-inflammatory proteins and downregulating pro-inflammatory cytokines. This is crucial when co-managed with orthobiologics, which depend on orchestrated inflammation for regenerative messaging.
- Microcirculation and Lymphatics
-
- PBM improves capillary perfusion, enhances oxygen delivery, and accelerates lymphatic clearance, reducing edema and clearing algogenic biochemicals (bradykinin, prostaglandins).
- Neuromodulation
-
- Reduces peripheral sensitization via membrane stabilization and improved neuronal metabolism. Facilitates central dampening of pain via decreased peripheral nociceptive input.
- Repair and Remodeling
-
- Stimulates fibroblast activity and collagen maturation, reorganizes the ECM, and supports angiogenesis, thereby accelerating wound closure and tendon-ligament healing.
Indications and Protocols: Practical Application Across Conditions
- Musculoskeletal Pain and Dysfunction
-
- Tendinopathies and Enthesopathies: Target insertional points point-by-point; 8–12 sessions for chronic cases, 2–3 weekly. Rationale: mitochondrial upregulation, cytokine modulation, ECM remodeling, microvascular perfusion.
- Osteoarthritis (Knee, Hip, Spine): Scan joint lines with robotic uniformity; dose both anterior and posterior compartments when feasible. PBM reduces synovial inflammation, enhances cartilage metabolism (indirect), and improves pain/function metrics.
- Myofascial Pain and DOMS: Wide-field scanning to address fascial planes; photomechanical effects modulate ECM; photochemical ATP boost aids recovery.
- Post-Surgical Recovery and Implants
-
- MLS’s safety profile allows dosing over plates, rods, screws, and prostheses without thermal risk, supporting analgesia, edema control, and faster return to function.
- Wound Care and Burns
-
- Apply around the margins and across viable tissue; MLS accelerates granulation and re-epithelialization and indirectly mitigates infection burden via improved perfusion and immune signaling. Burns paradoxically benefit because dosing is thermally safe while enhancing repair.
- Neuropathic Pain and Diabetic Neuropathy
-
- Emerging devices (e.g., MIS/MIS-S) have EU MDR clearance for neuropathic pain, leveraging pulsed NIR to improve nerve metabolism and microvascular support. Protocols emphasize consistent dosing and monitoring for sensory changes and function gains.
- Sports Medicine and Performance
-
- PBM pre-habilitation and acute recovery: point dosing on high-load tendons and muscle bellies; scan patterns for large muscle groups. Outcomes include reduced DOMS, faster return to play, and improved functional readiness.
Dosing Schedules and Practical Implementation
- Session Duration
-
- Typical treatments range from 6 to 12 minutes per area, scaled by region size, depth, and pathology. Multi-regional treatments may be sequenced or performed concurrently with robotic arms.
- Frequency
-
- Acute: 4–6 sessions over 2–3 weeks.
- Chronic: 8–12+ sessions over 4–6 weeks.
- Adjust based on patient response, functional goals, and co-therapies (e.g., orthobiologics injection timing: pre-day-of to prime mitochondrial state; post-injection to modulate inflammatory resolution without suppression).
- Adjunctive Care
-
- Combine PBM with shockwave (mechanotransductive stimulus), orthobiologics (regenerative signaling), graded loading, sleep and nutrition protocols (omega-3, polyphenols), and breath/autonomic training to maximize outcomes.
Safety, Liability, and Workflow Considerations
- Thermal Safety
-
- MLS’s synchronized pulsed profile prevents temperatures from exceeding ~43°C, thereby avoiding inhibitory and harmful thermal ranges. Staff can perform point dosing.
- Consistency
-
- Robotic systems standardize dosing across operators, reducing variance and improving reproducibility.
- Efficiency
-
- Hands-free setups allow concurrent treatments or staff multitasking. Software interfaces automatically guide therapeutic dosing based on anatomical and pathological inputs.
- Economic and Practical Notes
-
- While integration often begins with patient-first clinical intent, practices may find PBM to be a profitable adjunct due to demand and outcomes. Pricing structures and protocol packages should align with ethical, outcome-driven care models and support transparent communication.
Evidence Base: Trials, RCTs, Registries, and Real-World Observations
- Randomized Controlled Trials and Clinical Studies
-
- Positive outcomes reported for plantar fasciitis, knee osteoarthritis, chronic neck pain, and other MSK conditions. Importantly, MLS demonstrates safe use over surgical implants and tattoos, differentiating it from many class IV lasers that carry thermal caution in these contexts.
- Wound Healing Case Series
-
- Before-and-after documentation shows accelerated closure in post-surgical wounds, infected wounds, burns, and diabetic ulcers following structured MLS protocols.
- Data Biologics Registry (24-Month Outcomes)
- Orthobiologics + MLS exhibited:
-
-
- Faster and greater reductions in numeric pain ratings.
- Lower worst pain trajectories sustained out to 24 months.
- Higher desired functionality gains crossing early and widening over 1–6 months.
- High patient satisfaction (~96% long-term).
- Case volume >6,800 across diverse clinics suggests generalizability.
-
-
-
-
- Interpretation: PBM synergizes with biologics to amplify early analgesia and functional acceleration while sustaining improvements—consistent with mitochondrial and inflammatory modulation models.
-
-
Integrative Clinical Observations: Insights from Practice and HealthVoice360
- Patient-Centric Application
- In my clinical experience, integrating PBM into regenerative protocols improves early-phase comfort, enabling earlier movement, better adherence to graded activity, and reduced reliance on analgesics. HealthVoice360 case narratives mirror these findings—patients often report faster transitions from pain-limited to function-forward states when PBM is layered appropriately.
- Mitochondrial Health as a Foundational Strategy
- PBM adds a cellular energy axis to care plans. When paired with nutrition, sleep, and stress regulation, the bioenergetic improvements compound, fostering resilient tissue adaptation.
- Tissue-Specific Adjustments
- Tendon, joint, and nerve dosing differ in focal strategy, session count, and follow-up progression. Software guidance assists, but clinician reasoning remains vital—consider depth, vascular supply, comorbidity, and implant presence.
- Autonomic and Vascular Dynamics
- Patients with autonomic dysregulation (e.g., chronic pain syndromes) often benefit from PBM’s gentle modulation—routinized sessions reduce sympathetic drive via pain reduction and increased movement confidence.
- Workflow and Operations
- Robotic MLS improves staff utilization and standardization—especially valuable in multi-provider practices. Hands-free operation facilitates concurrent therapies and patient education, increasing overall throughput without compromising the quality of care.
Advanced Physiologic Discussion: Why Each Technique Is Used and the Logic of Protocols
- Point-by-Point for Focal Pathologies
- Rationale: Concentrated dosing maximizes J/cm² at the lesion, critical for entheses/tendon insertions with limited vascularity. Pulsed 905 nm ensures deep photon delivery without heat accumulation. Expected outcomes: decreased local cytokine load, improved fibroblast kinetics, enhanced collagen alignment.
- Scanning for Diffuse Myofascial Patterns
- Rationale: Distributed dosing across planes modulates widespread ECM tension and nociceptive fields. Robotic uniformity minimizes human error, maintains consistent photon density throughout the area, and supports global improvements in perfusion.
- Robotic Automation
- Rationale: Eliminates operator variability; ensures reproducible dosing linked to the anatomy and pathology phase. Facilitates multi-modal sessions and adherence to protocolized energy delivery. Expected outcomes: improved consistency across patient cohorts and better long-term metrics.
- Pulsed vs. Continuous Considerations
- True pulsing at nanosecond scales enables thermal off periods, which are crucial for avoiding inhibitory temperature zones. Chopped continuous may delay heat build-up, but does not fully prevent it—MLS’s synchronized pulsing is therefore preferred for safety and stronger biologic effects.
- Orthobiologics Synergy
- Rationale: PBM enhances mitochondrial ATP—supporting regenerative cell activity; modulates inflammatory signals without suppressing them. Timing PBM around injections (pre-day-of and post-injection) can prime tissue energetics and support organized resolution, improving clinical trajectories.
- Shockwave + PBM
- Rationale: Shockwave offers mechanotransductive microtrauma and angiogenic stimulation; PBM complements by enhancing ATP, NO, and vascular perfusion, improving tolerance, and accelerating repair scaffolding. Together, they address both mechanical and bioenergetic domains.
Condition-Specific Rationales and Protocol Examples
- Knee Osteoarthritis
- Targets: Synovium, capsular structures, periarticular soft tissue.
- Dosing: Robotic scan anterior/posterior compartments; 8–12 sessions; 2–3 per week.
- Rationale: Reduce synovitis, improve microcirculation, modulate nociception, support functional gains.
- Plantar Fasciitis
- Targets: Proximal fascial insertion at calcaneus; hands-free focal dosing; 6–10 sessions.
- Rationale: Decrease local inflammation, support collagen remodeling, and alleviate nociceptive signaling.
- Chronic Neck Pain
- Targets: Deep paraspinals, facet capsules; careful windowing to avoid high-reflection bony ridges.
- Rationale: PBM reduces myofascial hypertonicity, modulates facet-related nociception, and enhances perfusion.
- Post-Operative Care (with Implants)
- Targets: Peri-incisional tissues, deep soft tissues surrounding prostheses.
- Rationale: Analgesia without heat risk; improved lymphatic clearance; faster functional rehabilitation.
- Diabetic Foot Ulcers
- Targets: Peri-wound margins; adjust energy density to tissue tolerance; frequent early sessions.
- Rationale: Angiogenesis support, improved granulation, and modulation of local inflammatory milieu.
- Neuropathic Pain
- Targets: Nerve pathways and distal target fields; consistent pulsed dosing; monitor sensory function.
- Rationale: Improved axonal metabolism, perfusion, and nociceptor stabilization; supports neuroplastic recalibration.
Operationalizing MLS in Practice: Implementation Steps
- Assessment
- Comprehensive exam to identify pain generators, tissue depth, vascular status, and comorbidities. Map target zones and windowing paths.
- Protocol Selection
- Use software guidance for J/cm² baselines; modify based on chronicity and patient sensitivity. Determine point-by-point vs. robotic scanning.
- Scheduling
- Establish treatment cadence. For chronic cases, consider front-loading sessions (e.g., three times weekly initially) to accelerate early gains, then taper.
- Integration
- Align PBM with manual therapy, corrective exercise, shockwave, and orthobiologics. Educate patients on the cumulative nature and expectations.
- Monitoring
- Track pain scores, functional measures, and qualitative markers (sleep, activity tolerance). Adjust dose parameters iteratively.
Clinical Pearls and Practical Tips
- Depth Matters: Favor 905 nm pulsed emphasis for deeper structures; maintain synchronized 808 nm for mitochondrial priming across layers.
- Bone Reflection: Target joint spaces and soft-tissue corridors; avoid prolonged, stationary dosing directly over dense bone without windowing.
- Implant/Tattoo Safety: MLS’s profile supports safe dosing; still observe standard precautions and patient feedback.
- Cumulative Strategy: Reinforce to patients that benefits accrue over the course of sessions; set realistic timelines.
- Adjunctive Lifestyle: Encourage anti-inflammatory nutrition, hydration, sleep hygiene, and graded movement for synergistic outcomes.
Research Integration and Thought Leadership
- Leading Researchers’ Findings
- Contemporary PBM literature underscores cytochrome c oxidase activation, controlled ROS signaling, and NO-mediated vasodilation as core mechanisms. Trials demonstrate improvements across pain scales and functional outcomes with appropriate dosing. Registry data confirm real-world reproducibility and long-term sustainability of benefits—especially when PBM is integrated with biologics.
- Modern Methods
- Trials, RCTs, and registries provide multi-modal evidence: mechanistic (biochemical assays), clinical endpoints (pain, function), and systems-level outcomes (return to activity, satisfaction). MLS’s synchronized emission represents a methodologically distinct approach—leveraging physics to achieve biologic precision.
Extended Clinical Integration: From Protocols to Pathways
- Pre-Injection PBM
- Rationale: Optimize mitochondrial readiness; reduce baseline pain to improve injection tolerance; enhance local perfusion.
- Post-Injection PBM
- Rationale: Support organized inflammatory resolution, augment cellular energetics, and stabilize nociceptive signaling without suppression.
- Performance Medicine
- Use PBM to maintain tissue readiness across training cycles; shift dosing toward recovery phases to reduce DOMS and sustain training volume.
- Chronic Pain Programs
- Combine PBM with CBT or pain education, graded exposure, and autonomic regulation (breath, HRV). PBM’s analgesia facilitates engagement in functional rehab.
Workflow Efficiency and Quality Assurance
- Standardization
- Utilize robotic dosing for consistency; document energy delivery, session parameters, and clinical responses.
- Safety Checklists
- Eye protection, device calibration, skin inspection, and patient feedback loops.
- Outcome Tracking
- Pain scores, functionality indices, satisfaction metrics. Benchmark against registry data where possible.
Ethics, Economics, and Patient Communication
- Ethics
- Emphasize evidence-based dosing, transparency about the cumulative nature, and realistic expectations.
- Economics
- PBM can be cost-effective and scalable. Align pricing with outcome-oriented packages (acute vs. chronic) and reinforce value via documented progress.
- Communication
- Explain PBM mechanisms: “We are energizing cells, improving blood flow, and calming pain signals without drugs or heat damage.” Use analogies (photosynthesis, synchronized wavefronts) to improve understanding.
Case Vignettes and Outcome Narratives (Representative)
- Chronic Knee OA with Biologics
- Integrated PBM reduced pain more quickly than biologics alone; improved gait speed within 3 weeks; sustained gains at 6 months.
- Plantar Fasciitis in a Recreational Runner
- Point dosing at proximal fascia; pain improved by session 4; return to run by week 3 with shockwave adjunct.
- Post-Op TKR with Implant
- Safe dosing over prosthesis; edema reduced; faster ROM gains; discharged from rehab earlier than typical benchmarks.
- Diabetic Foot Ulcer
- MLS added to standard wound care; granulation accelerated; ulcer area reduced substantially over 8–10 treatments.
- Neuropathic Pain
- Consistent pulsed dosing; improved light touch/cold discrimination; decreased burning over 6 weeks; activity tolerance increased.
Future Directions and Innovation
- Device Evolution
- Portable MLS units (battery-powered) enable field/trainer use, expanding access and continuity of care.
- Neuropathy Focus
- MDR-cleared EU devices indicate expanding regulatory acceptance; ongoing US adoption expected.
- Aesthetic and Dermal Applications
- Address complications (e.g., post-procedural inflammation) with controlled PBM to improve recovery profiles.
Keywords
Photobiomodulation, MLS laser therapy, multiwave locked system, 808 nm, 905 nm, pulsed emission, mitochondrial function, cytochrome c oxidase, nitric oxide, ROS signaling, vasodilation, lymphatic drainage, extracellular matrix, mechanotransduction, osteoarthritis, tendinopathy, neuropathic pain, wound healing, burns, implants, tattoos, shockwave synergy, orthobiologics, regenerative medicine, robotic laser, hands-free therapy, energy dosing, J/cm², Data Biologics registry, pain modulation, functional outcomes.
References
- Leading PBM and MLS research publications on cytochrome c oxidase activation, NO-mediated vasodilation, and clinical outcomes in MSK disorders, neuropathy, and wound healing.
- Randomized controlled trials demonstrate the multi-wavelength of class IV synchronizemulti-wavelengthth PBM for plantar fasciitis, knee osteoarthritis, and chronic neck pain.
- Data Biologics registry reports (24-month outcomes) on orthobiologics combined with MLS laser therapy, including pain reduction, functional improvement, and patient satisfaction trends.
Note: For specific citation lists or to access study PDFs organized by indication (OA, tendinopathy, neuropathy, wound care), contact our clinical support team. The studies cited above encompass randomized controlled trials, cohort analyses, mechanistic investigations, and registry data.
Disclaimers
- The content provided is for educational purposes only and should not be used as medical advice.
- All individuals must obtain recommendations for their personal situations from their own medical providers.
Summary
I outlined a modern, integrative framework for photobiomodulation (PBM) with MLS Robotic Laser Therapy, emphasizing evidence-based physiology, dosing science, safety, and real-world clinical outcomes. PBM operates within the 600–1200 nm therapeutic window to trigger photochemical, photothermal, and photomechanical effects. Its central mechanism involves cytochrome c oxidase activation, increased ATP production, nitric oxide-mediated vasodilation, and carefully modulated ROS signaling. MLS laser therapy—synchronizing 808 nm continuous emission with 905 nm pulsed emission—achieves class IV efficacy while maintaining class III-like safety, thanks to true pulsing and thermal relaxation that prevent crossing inhibitory or damaging temperature thresholds. This design produces homogeneous energy distribution, improved photon density at depth, and precise dosing capacity.
Clinically, MLS addresses pain, inflammation, microcirculation, lymphatic drainage, ECM remodeling, and neural stabilization across musculoskeletal disorders, post-surgical recovery (including over implants), wound care (including burns and diabetic ulcers), neuropathic pain, and sports performance. Techniques include point-by-point dosing for focal lesions and robotic scanning for broader fields, with software-guided, anatomically driven parameters ensuring consistent J/cm² delivery. PBM integrates seamlessly with shockwave and orthobiologics, modulating inflammation rather than suppressing it—an essential characteristic for regenerative synergy. Protocols typically span 4–6 sessions for acute issues and 8–12 for chronic conditions, delivered 2–3 times weekly.
Evidence includes RCTs for plantar fasciitis, knee OA, and chronic neck pain; case series in wound care; and Data Biologics registry data demonstrating faster pain reduction, improved functional indices, and sustained benefits at 24 months when MLS is combined with biologics. Safety advantages extend to dosing over implants and tattoos, uncommon among class IV lasers. Operational benefits—robotic hands-free delivery, workflow efficiency, and standardized dosing—support high-quality, reproducible care. From HealthVoice360 clinical observations, integrating PBM into comprehensive plans enhances early comfort, accelerates functional rehabilitation, and reduces reliance on analgesics.
Conclusion
MLS laser therapy represents a mature, physiologically coherent, and clinically validated approach to improving cellular energetics, modulating inflammation, and accelerating repair. By synchronizing multi-wavelength emissions and leveraging true pulsing, MLS delivers deep, effective doses while preserving safety—making it ideal for focal musculoskeletal lesions, diffuse pain fields, post-operative regions with implants, chronic neuropathic conditions, and wound healing. When embedded in integrative pathways—orthobiologics, shockwave, manual therapy, graded loading, nutrition, and sleep—MLS contributes to superior patient outcomes, early functional gains, and sustained improvements.
Key Insights
- Photobiomodulation’s value lies in optimizing mitochondrial ATP production, vascular dynamics, and ECM remodeling while modulating inflammatory signals.
- MLS’s synchronized 808/905 nm architecture achieves class IV efficacy with class III-like safety through true pulsing and thermal relaxation.
- Robotic hands-free delivery standardizes dosing, improves workflow, and enables precise point-by-point or uniform scanning protocols.
- Clinical evidence and registry data support faster pain relief, better functional outcomes, and high patient satisfaction, especially when MLS is integrated with orthobiologics.
- Ethical, transparent implementation, patient education, and adjunctive lifestyle strategies amplify PBM’s impact across diverse conditions.
Disclaimers
- The content provided is for educational purposes only and should not be used as medical advice.
- All individuals must obtain recommendations for their personal situations from their own medical providers.
General Disclaimer
Professional Scope of Practice *
The information herein on "MLS Laser Therapy & Photobiomodulation for Pain Relief in the Body" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics