Table of Contents
Introduction
The body is always going through many factors that constantly test the durability that can affect the entire microbiome itself. The gut helps the body’s homeostasis by metabolizing the nutrients that provide the energy for functionality. The gut system is home to trillions of microorganisms that communicate to the brain system, endocrine system, immune system, and skin to ensure that it is healthy. When disruptive factors enter the gut system, they can cause various issues that can make the dysfunctional body while affecting its communication with the body’s axis. Today’s article focuses on a skin condition that everyone has suffered in their lives known as acne and how the gut-skin axis is being affected by acne. Referring patients to certified, skilled providers who specialize in gastroenterology treatments. We provide guidance to our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is critical for asking insightful questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
What Is Acne Vulgaris?
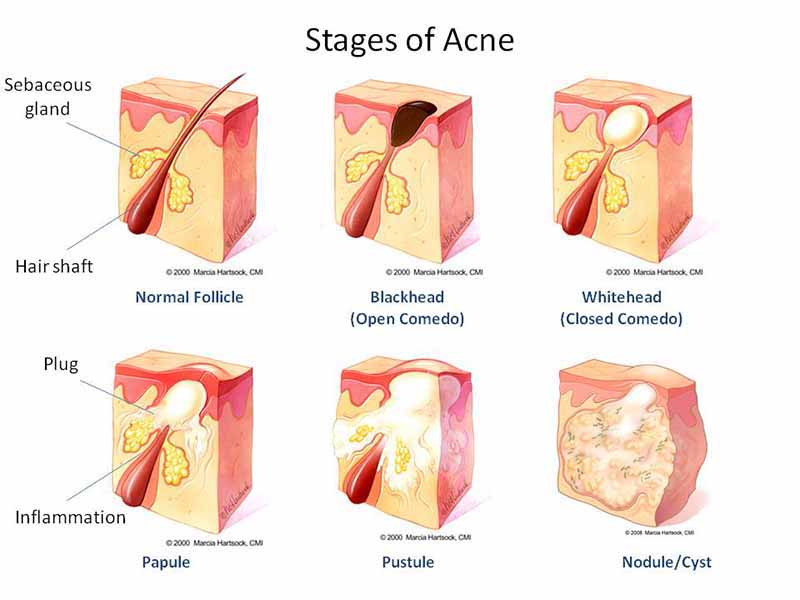
Have you noticed bumps along your face, especially in the nose, forehead, and cheek regions? How about inflammatory reactions that are affecting your skin? Do issues like GERD, IBS, leaky gut, or SIBO affect your gut? Most of these issues are due to disruptive factors that affect the gut-skin connection and cause a skin condition known as acne vulgaris. Everybody suffers from acne when they are young, and it is a common condition with follicular papules or comedones and inflammatory papules and pustules. Research studies have shown that acne vulgaris is an inflammatory disorder triggered by many factors that can cause it to become aggravated and inflamed. Some of the contributing factors that can cause acne vulgaris to form due to the following:
- Infection (Propionibacterium acnes)
- Tissue inflammation
- Plugging of hair follicles due to epidermal hyperproliferation
- Hormone imbalance
- Endocrine disorders
- Excess sun exposure
Other research studies have shown that other factors like gut disorders can also affect the development of acne vulgaris. Acne vulgaris can be associated with the emotional factors that affect the brain and the gut’s inflammatory factors as they go hand in hand. When a person becomes stressed or anxious, their skin will flare up and develop acne around some skin regions. Additional studies have mentioned that emotional factors like stress and anxiety can alter the gut microbiota and increase intestinal permeability. When gut disorders start to contribute to skin inflammation, it can aggravate acne to develop and form on the skin.
Gut Health & Acne- Video
Have you experienced gut disorders that seem to affect your quality of life? Have you noticed that particular foods you consume are not sitting well in your gut system? How about feeling overly stressed and anxious that acne forms around your face? The video above explains how the gut microbiome affects a person when making dietary changes that can provide beneficial results to the gut microbiota. Research studies have found that the intestinal microbiota is essential for forming acne lesions while being responsible for proper immunity and defense of the microorganisms. The GI tract and acne condition are closely associated because they provide the neuroendocrine and immune functions to the body.
The Gut-Skin Axis & How It Affects Acne
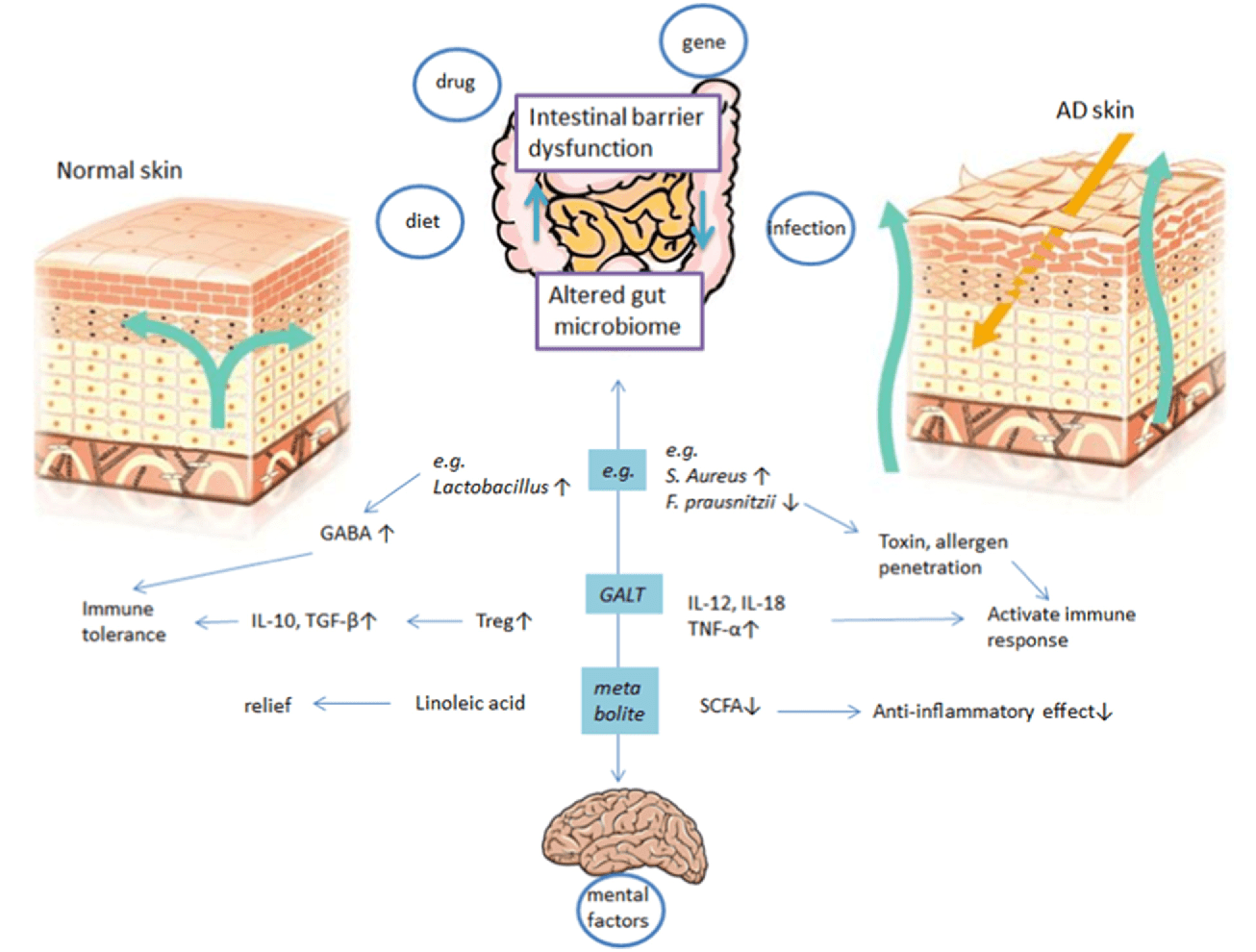
Since the gut is the host to trillions of bacteria, its primary job is to maintain constant communication with the skin to dampen unnecessary inflammatory markers that can cause the skin to break out. Research studies have found that the gut-skin axis, when affected by acne, produces significantly higher metabolites that generate ROS (reactive oxygen species) and induce inflammation in both the gut and skin. Additional research has shown that the gut microbiome plays an essential role in skin disorders and vice versa. When changes affect either the gut or the skin, it can drastically change a person’s outcome in life. Say, for instance, dietary habits that cause inflammation in the gut. This is due to processed foods that cause the gut to become inflamed and make the skin begin the development of acne in different portions of the skin. Research shows that the gut microbiome can vastly influence the immune system by regulating it. This builds a tolerance to dietary changes in the gut to promote acne-free skin. So incorporating a low-glycemic-load diet has been linked to improved acne, possibly through gut changes or attenuation of insulin levels.
Conclusion
Overall, the gut plays a massive role in the body in its homeostasis as it helps the body metabolize the nutrients to keep it functioning and moving. The gut microbiota also has bidirectional communication with the skin as common skin disorders like acne tend to show up. Acne is very common amongst individuals, especially in younger individuals, as it can affect their moods and cause changes to their mental health and their gut health. Incorporating small changes like eating healthy food, maintaining a stress-free environment, and even exercising can help not only lower gut inflammation but also clear up the skin from acne.
References
Bowe, Whitney P, and Alan C Logan. “Acne Vulgaris, Probiotics and the Gut-Brain-Skin Axis – Back to the Future?” Gut Pathogens, BioMed Central, 31 Jan. 2011, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3038963/.
Chilicka, Karolina, et al. “Microbiome and Probiotics in Acne Vulgaris-A Narrative Review.” Life (Basel, Switzerland), MDPI, 15 Mar. 2022, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8953587/.
De Pessemier, Britta, et al. “Gut-Skin Axis: Current Knowledge of the Interrelationship between Microbial Dysbiosis and Skin Conditions.” Microorganisms, MDPI, 11 Feb. 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7916842/.
Lee, Young Bok, et al. “Potential Role of the Microbiome in Acne: A Comprehensive Review.” Journal of Clinical Medicine, MDPI, 7 July 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6678709/.
Salem, Iman, et al. “The Gut Microbiome as a Major Regulator of the Gut-Skin Axis.” Frontiers in Microbiology, Frontiers Media S.A., 10 July 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6048199/.
Sutaria, Amita H, et al. “Acne Vulgaris.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 8 May 2022, https://www.ncbi.nlm.nih.gov/books/NBK459173/.
Disclaimer
General Disclaimer
Professional Scope of Practice *
The information herein on "The Gut Microbiota Could Be The Source Of Acne" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics