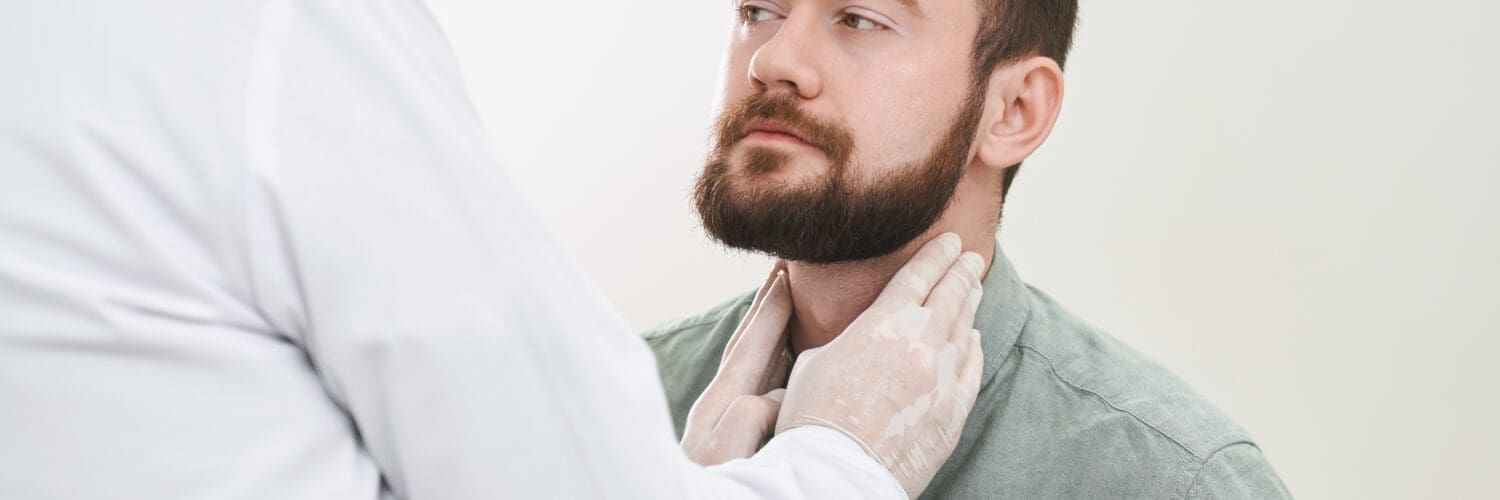
Discover the role of thyroid optimization for hormones in promoting wellness and energy levels for a healthier lifestyle.
Table of Contents
Introduction Abstract
I am Dr. Alexander Jimenez, DC, FNP-APRN. Over decades of clinical practice, research immersion, and continuous study, I have watched modern thyroid care evolve—sometimes faster than clinicians and patients can comfortably adapt to. This educational post distills what I have learned by pairing rigorous evidence-based methods with the day-to-day realities I witness and document in my clinic and at HealthVoice360.com. My dual vantage point—as a chiropractor and a family nurse practitioner—allows me to see endocrinology both through mechanistic physiology and whole-person systems thinking. This synthesis matters because a subset of individuals remain symptomatic under standard hypothyroidism management despite “normal labs,” especially a “normal” thyroid-stimulating hormone (TSH). My goal is to connect the dots between lab numbers and lived outcomes and to fully explain, in a narrative first-person format, the why behind each evaluation and therapy choice.
In the sections that follow, I explain how thyroid hormones move from the gland to the blood to the cell nucleus to the mitochondria, and why free T3 (the active thyroid hormone) often correlates best with patient function. I discuss deiodinase enzymes (DIO1, DIO2, DIO3), transporter dynamics (such as MCT8/MCT10), receptor coactivators, and inflammatory and stress signals that divert T4 toward reverse T3 (rT3) and away from T3. I clarify why TSH alone cannot capture tissue-level sufficiency in treated patients; the pituitary’s privileged conversion environment (dominant DIO2) can normalize or suppress TSH even as peripheral tissues remain T3-deficient. I explore the clinical patterns I see repeatedly in practice—Type 1 (low production), Type 2 (conversion deficit with rT3 elevation), and Type 3 (receptor insensitivity)—and why identifying these patterns shifts care from a single-marker paradigm to a mechanism-first model.
You will find a thorough explanation of combination therapy (LT4+LT3) and desiccated thyroid extract (DTE), including dosing logic, safety monitoring, and lab timing discipline to prevent misinterpretation of post-dose peaks. I present operational details for split dosing (BID/TID), iron/ferritin repletion, selenium and zinc, and careful iodine strategies that respect sodium-iodide symporter (NIS) biology and halogen competition. I describe the role of insulin resistance, sleep architecture, autonomic balance, and training (resistance and Zone 2 aerobic) in resetting conversion capacity and mitochondrial execution of thyroid signals. I also integrate the cross-talk with testosterone and sex hormones, explain why certain medications and stressors disrupt conversion, and show how correcting confounders (e.g., ferritin <50 ng/mL, sleep apnea) often unlocks thyroid therapy without escalating doses.
Because safety is paramount, I delineate cardiovascular and bone guardrails, how I interpret suppressed TSH under therapy, and why free hormone levels and clinical state matter more than the pituitary’s solitary voice. I share case narratives—drawn from my practice and aligned with observations at HealthVoice360—that illustrate the transformation many patients experience when therapy is individualized, and labs are timed consistently. The post culminates in practical algorithms, lab panels, dosing strategies, and clinic workflows that standardize care and improve reproducibility. It closes with references, keywords, and a comprehensive summary, conclusion, and key insights.
This is not a lecture; it is an educational web post designed to be read, revisited, and applied. I have written it in a narrative style so readers can follow the clinical reasoning from physiology to protocol, understand why each technique or idea exists, and see how modern, evidence-based research methods and leading investigator findings translate into outcomes that patients can feel every day. My objective is simple: honor mechanisms, personalize care, and align therapy with real-world physiology and safety. When we do that, the gap between “normal labs” and “normal life” begins to close.
Why Normal TSH Does Not Guarantee Normal Life
When I sit with a patient who says, “I don’t feel right,” even though their TSH is “normal,” I begin with physiology. TSH is an upstream pituitary signal; it indicates what the pituitary thinks the circulating thyroid hormone levels are. But thyroid hormone action—what creates energy, warmth, bowel motility, cognitive speed, and metabolic tone—occurs inside tissues, mediated by free T3 binding to nuclear receptors (TR?, TR?) and driving gene transcription. There is a fundamental mismatch between a single central signal and the myriad requirements of peripheral tissues.
- The pituitary efficiently converts T4 to T3 via DIO2, often maintaining its own local T3 sufficiency even when peripheral tissues struggle. This can normalize or suppress TSH, masking a systemic T3 deficit.
- Under illness, chronic stress, or inflammation, peripheral deiodinase balance shifts toward DIO3—increasing rT3, which occupies receptors without activating metabolism. That produces a “functional hypothyroid” state in tissues despite “normal” TSH.
- Many patients on LT4 monotherapy have normal free T4 and TSH, but free T3 is low-normal, and rT3 is elevated. Clinically, they present with cold intolerance, fatigue, constipation, dry skin, brittle nails, hair thinning, cognitive fog, and weight gain or resistance to weight loss. This pattern, a Type 2 conversion deficit, is common.
In my practice, acknowledging this mismatch is the first step. I widen the lens beyond TSH. I order free T4, free T3, rT3 when indicated, thyroid antibodies (TPOAb, TgAb), iron and ferritin, selenium and zinc, vitamin D and B12, magnesium, hs-CRP, fasting insulin and A1c, lipid profiles, liver/kidney function, and sex hormones when clinical context suggests cross-axis effects. I also evaluate sleep quality, circadian rhythm, autonomic balance, and body composition. The “why” behind each test is mechanistic: each marker identifies a lever we can pull to restore conversion and receptor-level action.
A Personal Lens on Profound Hypothyroidism
My perspective is shaped by deep lived experience. I have seen many patients undergo periods of profound hypothyroidism to drive TSH very high during diagnostic withdrawal phases. At TSH >150 mIU/L, I felt what true cellular energy deprivation means when treating them: severely slowed bowel transit with virtually no spontaneous movements, cognitive haze so dense it distorted time perception, a body struggling to thermoregulate, muscles fatiguing under trivial loads, and skin losing its natural luster.
While caring for thousands of patients in my integrative chiropractic practice has made the duality clear, I respect clinical guidelines and their limitations. In practice, I routinely witness the full spectrum of thyroid imbalance. Patients often describe classic hypothyroid effects such as debilitating fatigue, cold intolerance, constipation, weight gain, brain fog, slowed cognition, low mood or depression, hair thinning, dry skin, muscle weakness, and exercise intolerance. Others experience disruptive hyperthyroid manifestations, including unintended weight loss despite increased appetite, heat intolerance, anxiety or irritability, rapid heartbeat or palpitations, diarrhea, tremors, restlessness, insomnia, and excessive sweating.
That visceral understanding taught me to respect what thyroid hormones truly do—not merely as lab values, but as a human felt reality. The lesson is simple: when I listen carefully to the patient and their individual physiology, supported by precise chiropractic adjustments that optimize spinal alignment, nervous system function, and autonomic balance, therapy becomes safer and far more effective. If I listen only to a single marker, I risk missing the complete tissue-level story.
Environmental Radiation, Autoimmunity, and The Thyroid Vulnerability
The thyroid concentrates iodine and is uniquely vulnerable to radiation and environmental disruption. In my clinic, I consider the environmental backdrop alongside autoimmunity and nutrient status:
- Autoimmunity: Hashimoto’s thyroiditis is prevalent in iodine-sufficient regions. Elevated TPO and Tg antibodies indicate immune activation. Flares can relate to infections, diet, stress, and environmental toxins.
- Iodine dynamics: Both deficiency and excess can destabilize thyroid autoimmunity. Contextual dosing with selenium support mitigates risk.
- Toxin burden: Perchlorates, thiocyanates, and endocrine-disrupting chemicals interfere with iodine uptake and synthesis.
- Nutrient deficits: Selenium, iron/ferritin, zinc, vitamin A, and vitamin D impair synthesis, conversion, and receptor function.
- Inflammation: Cytokine-rich milieus upregulate DIO3 and downregulate DIO1/DIO2, reducing tissue T3.
Each of these factors shifts deiodinase balance or receptor coactivator function. By addressing them, standard therapy regains traction. I see this routinely: iron repletion, selenium and zinc support, anti-inflammatory nutrition, and sleep restoration reduce rT3 and elevate free T3 without dose escalation.
From Gland to Gene—The Full Itinerary of Thyroid Hormone Action
To explain persistent symptoms, I trace hormone flow step by step:
- Synthesis and secretion: The thyroid produces mostly T4 and smaller amounts of T3. T4 is a prohormone; tissues activate it to T3.
- Transport: Hormones circulate bound to TBG, albumin, and transthyretin; only the free hormone acts immediately.
- Cellular uptake: Transporters such as MCT8/MCT10 and OATP facilitate the uptake of thyroid hormones into cells. Polymorphisms or inflammatory downregulation reduce intracellular T3 even when serum levels look adequate.
- Conversion: Do DIO1/DIO2 activate T4? T3; DIO3 inactivates (T4 ? rT3, T3 ? T2). Stress and inflammation tilt the balance toward inactivation.
- Receptor binding: Free T3 binds TR?/?, recruiting coactivators and modifying chromatin to transcribe T3-responsive genes controlling mitochondrial biogenesis, oxidative phosphorylation, ion channel density, lipolysis, and thermogenesis.
- Mitochondrial execution: T3 increases mitochondrial density, UCPs, and ATP. Without cofactors (iron for cytochromes, selenium for deiodinases and glutathione peroxidases, CoQ10, B vitamins, and magnesium), cells cannot execute the transcriptional program.
If any step falters—transport, conversion, receptor coactivation, mitochondrial response—the patient can feel hypothyroid despite “normal” bloodwork.
Why Levothyroxine (LT4) Alone Sometimes Falls Short
LT4 monotherapy is standard and helps many. However, I routinely meet patients whose labs normalize while they remain symptomatic. The physiology explains why:
- Suboptimal conversion: Genetics (e.g., DIO2 polymorphisms), inflammation, nutrient deficits blunt DIO1/DIO2.
- Transporter issues: Impaired MCT8/MCT10 reduces cellular T3 entry despite normal serum levels.
- Increased DIO3 activity: Chronic stress and illness shunt toward rT3, inactivating T3 action.
- TBG shifts: Estrogen increases TBG, complicating the interpretation of free vs. total.
- Receptor milieu: Inflammatory cytokines alter receptor coactivator complexes, blunting T3’s genomic impact.
- Mitochondrial limits: Without micronutrients or sufficient caloric quality, the cell cannot translate T3 signals into energy.
Clinically, I see improved outcomes when we restore conversion capacity (iron, selenium, zinc, vitamin D), reduce inflammation, optimize sleep and insulin dynamics, and, in select cases, add a small physiologic dose of T3. This is not about abandoning LT4; it is about tailoring therapy to the mechanism.
Thyroid Dysfunction-Video
Combination Therapy Rationale and Safety Protocols
I approach LT4+LT3 or DTE carefully, guided by evidence and safety:
- Rationale: The thyroid secretes both T4 and T3. For patients with persistent symptoms and mechanistic evidence of conversion failure (low free T3, elevated rT3), physiological T3 provision can correct intracellular deficits.
- Method: I start low and slow—often 5–5 mcg LT3 once or twice daily—paired with a modest reduction in LT4 to avoid supraphysiologic exposure. Split dosing respects T3′s shorter half-life and peak kinetics.
- Monitoring: I track TSH, free T4, free T3, and consider rT3 when conversion is suspect. I watch for palpitations, anxiety, insomnia, and heat intolerance, and monitor bone and cardiac risks. I employ functional metrics—fatigue scales, bowel diaries, grip strength, 6-minute walk, HRV—and schedule rechecks at 6–8 weeks to gauge both labs and function.
I explain these steps to patients up front. Informed expectations and transparent guardrails reduce anxiety and improve adherence.
Desiccated Thyroid Extract—Patient-Reported Benefits and Practical Cautions
DTE delivers T4, T3, and other iodothyronines. Many patients report improved well-being on DTE or combination therapy. Possible reasons:
- Direct T3 provision bypasses conversion bottlenecks.
- Additional iodothyronines (e.g., T2) may exert mitochondrial effects (under investigation).
- Kinetics produce transient T3 peaks that alleviate symptoms for some.
Cautions: DTE’s T4:T3 ratio is lower than that of humans; careful dosing and monitoring are required. Historically, batch variability raised concerns, but modern standards have improved consistency. When I use DTE, I equate doses to rational T4/T3 exposures, assess responses, and adjust thoroughly.
The Weight Puzzle—Why Normalizing TSH Doesn’t Automatically Normalize Weight
One of the most frustrating gaps is body weight. Many patients on LT4 struggle with weight despite normal labs. Reasons:
- Metabolic adaptation: Chronic hypothyroidism and repeated dieting lower resting energy expenditure (REE). Restoring euthyroidism may not fully reverse adaptive thermogenesis.
- Inflammation: Adipose inflammation blunts deiodinases (DIO1/DIO2) and receptor coactivators; DIO3 rises, reducing tissue T3.
- Insulin resistance: Hyperinsulinemia drives lipogenesis and suppresses lipolysis; it also interferes with thyroid receptor signaling and mitochondrial output.
- Sleep and circadian disruption: Lower insulin sensitivity, altered leptin/ghrelin, increased appetite.
- Sarcopenia: Lower lean mass reduces basal metabolic rate and glucose disposal, trapping metabolism.
- Medications: Beta-blockers, certain antidepressants, and antipsychotics reduce metabolic tone.
I address these systematically: high-quality protein intake, structured resistance training, Zone 2 aerobic work, sleep optimization, insulin sensitivity, micronutrient sufficiency, and inflammation control. Weight responds when thyroid care is embedded within metabolic care.
Obesity Trends—Thyroid as a Potentiating Factor
Obesity has climbed dramatically over recent decades. Thyroid dysfunction is not the primary cause, but it is a potentiator:
- Even mild T3 deficits reduce thermogenesis, physical activity tolerance, and satiety signals.
- In an obesogenic environment, small hormonal nudges produce large population effects.
I integrate thyroid and metabolic care—insulin sensitivity, hepatic fat reduction, training—so therapeutic gains translate into body composition improvements.
Testosterone-Thyroid Cross-Talk and Clinical Implications
Endocrine axes converse. In men, hypothyroidism can lower gonadotropin signaling and testosterone synthesis; low testosterone reduces muscle mass and metabolic rate, worsening hypothyroid symptoms. In women, androgen balance affects SHBG, TBG, and free fraction dynamics; PCOS often travels with insulin resistance and thyroid autoimmunity.
I assess total/free testosterone, LH/FSH, SHBG, and related markers when appropriate. Addressing androgen status—starting with lifestyle and pharmacologic interventions when indicated—often synergizes with thyroid optimization, leading to improved lean mass, insulin sensitivity, mitochondrial function, and clinical resilience.
Precision Diagnostics—Beyond TSH
My core panel includes TSH, free T4, and free T3. When Hashimoto’s is suspected, I add TPOAb and TgAb. In persistent cases with stress/inflammation, I consider rT3. I evaluate iron/ferritin (hair and thyroid function often improve when ferritin reaches 50–100 ng/mL), selenium, zinc, vitamin D, B12, magnesium; I create a metabolic panel (fasting glucose/insulin, A1c, lipids, ALT/AST), and review cortisol patterns when sleep or stress are prominent. I use DEXA or bioimpedance for body composition, and Ean CG if adding T3 in cardiac-risk contexts.
Every test ties to a mechanism we can modify. Lab strategy is a map; therapy follows the terrain.
Nutritional Foundations—Fueling the Biochemical Machinery
Without cofactors and substrate, increasing hormone levels is like pressing a gas pedal with no fuel. I build:
- Protein: 1.2–1.6 g/kg/day to support lean mass and mitochondrial enzymes.
- Selenium: 100–200 mcg/day for deiodinase function and antioxidant defense.
- Iron: Optimize ferritin and transferrin saturation; iron powers thyroid peroxidase and cytochromes.
- Iodine: Adequate but not excessive; titrate in autoimmunity and pair with selenium.
- Zinc: Supports receptor binding and immune balance.
- Vitamin D: Immune modulation and muscle function.
- Omega-3s: Lower inflammation; may improve deiodinase balance.
- Polyphenols: Antioxidant support for mitochondria (berries, cocoa, green tea).
- Glycemic control: Low-glycemic, fiber-rich diets improve insulin sensitivity and reduce adipose inflammation.
Patients feel the difference when these foundations are in place. Therapy sticks; energy stabilizes.
Exercise as a Hormone Sensitizer—Mitochondrial Upgrades
Training translates hormone signals into performance:
- Resistance training raises lean mass, GLUT4 expression, insulin sensitivity, resting metabolic rate, and myokine profiles that reduce inflammation.
- Zone 2 aerobic training improves mitochondrial density and fat oxidation and stabilizes autonomic balance.
- High-intensity intervals are used sparingly to elevate VO2max without overtraining.
Thyroid hormones set the transcriptional program. Exercise supplies the mechanical stimulus that turns transcription into reality.
Sleep, Stress, and The Deiodinase Switch
Chronic stress and sleep debt tilt DIO3 upward, shunting T4 toward rT3 and inactivating T3. Cortisol dysregulation lowers receptor sensitivity. I intervene:
- Sleep hygiene: Consistent timing, darkness, cool temperature, wind-down rituals, limited screens.
- Cognitive/somatic tools: Mindfulness, paced breathing, vagal maneuvers, balanced strength, and aerobic training.
- Clinical support: CBT-I for insomnia, treating sleep apnea, and managing pain generators.
Restoring circadian robustness rebalances deiodinase activity toward DIO2, improving tissue T3 levels.
Medication Interactions and Special Populations
Context determines dosing strategy:
- Estrogen therapy raises TBG; free hormone may drop despite normal total—adjust doses.
- Biotin interferes with immunoassays—hold before labs.
- Glucocorticoids suppress TSH and alter conversion—interpret carefully.
- Beta-blockers reduce peripheral conversion—balance risks/benefits.
- Pregnancy increases TBG and thyroid demand—use trimester-specific ranges and close monitoring.
- Aging shifts TSH set-points—adults are more sensitive to T3 excess; titrate conservatively.
- Cardiac disease: Start low, go slow, collaborate with cardiology.
These guardrails reduce complications and increase confidence for patients and clinicians alike.
Pattern Recognition—Who Benefits from a Broader Approach?
Patterns guide me:
- Persistent fatigue, cold intolerance, constipation, weight gain despite normal TSH/free T4 with low-normal free T3, elevated rT3, high hs-CRP or insulin.
- Hair loss/brittle nails with ferritin <50 ng/mL—improve after iron repletion plus stable thyroid dosing.
- Postpartum autoimmunity fluctuations—require dynamic dose management.
- Older patients with palpitations on T3—benefit from micro-dosing or LT4-only paired with lifestyle optimization.
I do not escalate doses reflexively. I correct mechanisms first, consider combination therapy when supported, and monitor safety relentlessly.
Therapeutic Algorithm—Stepwise, Mechanism-First Care
I use structured progression:
- Confirm diagnosis and rule out confounders: anemia, B12 deficiency, sleep apnea, depression, medication effects, chronic pain, and overtraining.
- Optimize LT4 for TSH and symptoms.
- Address conversion of selenium, iron/ferritin, zinc, and vitamin D; anti-inflammatory nutrition; and insulin sensitivity.
- Reassess at 6–12 weeks: if symptoms persist and mechanisms support, consider combination therapy.
- Trial LT4+LT3 or DTE: low-dose, careful titration, informed consent, safety monitoring.
- Integrate exercise/sleep optimization for mitochondrial/autonomic recalibration.
- Evaluate labs and functional outcomes; iterate or de-escalate.
- Long-term maintenance: periodic labs, bone and cardiac risk assessment, sustained lifestyle support.
This method minimizes risk and reveals the true drivers of symptoms.
Safety First—Avoiding Overtreatment
Excess thyroid hormone threatens bone and cardiovascular stability. My guardrails:
- Favor small T3 doses; split dosing.
- Maintain TSH within safe ranges unless oncologic suppression is indicated.
- Screen for AFib risk; monitor heart rate and blood pressure.
- Protect bone: calcium, vitamin D, resistance training, DEXA when indicated.
- Reassess the necessity of T3; taper when conversion and lifestyle restoration allow.
Therapeutic success is the alignment of labs, function, and safety—not a low TSH.
Communication and Expectation Management
I tell patients: “The right dose is the one that aligns your labs, your function, and your safety metrics.” We set 6–12 week timelines between changes, discuss expected sensations, and define red flags together. Clear communication turns therapy into a collaborative process.
Integrating Real-World Observations—HealthVoice360 Case Narratives
The patterns above mirror cases I document at HealthVoice360.com:
- Iron and selenium optimization before dose escalation.
- The outsized role of sleep apnea in stubborn hypothyroid presentations.
- Synergy between structured resistance training and improved thyroid symptomatology.
- The value of meticulous, compassionate iteration—not hurried dosing.
Healing is not linear. Real-world cases keep us honest and grounded.
Evidence from Leading Researchers—Key Threads
Contemporary literature supports:
- A subset of patients improves with LT4+LT3, particularly in the context of DIO2 polymorphisms or impaired conversion.
- Inflammation and illness shift deiodinase expression toward DIO3, lowering tissue T3 despite normal TSH.
- Mitochondrial function is the proximate effector of thyroid hormone action; nutrients and training modulate outcomes.
- Excess thyroid hormone elevates AFib and fracture risk; individualized, conservative dosing is essential.
- Multimodal interventions amplify therapeutic gains and reduce the need for dose escalation.
These threads inform cautious optimism about combination therapy and a strong emphasis on lifestyle and cofactors.
A Patient Journey—From Labs to Outcomes
A representative case: a 45-year-old on LT4 with TSH 2.1 mIU/L, free T4 mid-range, free T3 low-normal, persistent fatigue, constipation, and weight gain. Ferritin 18 ng/mL, vitamin D 22 ng/mL, hs-CRP elevated, HOMA-IR positive, sleep study shows mild apnea.
- Step 1: Iron and vitamin D repletion; anti-inflammatory, high-protein,n low-glycemic nutrition; treat sleep apnea; progressive resistance and Zone 2
- Step 2 (8 weeks): Energy improves; free T3 remains low-normal; rT3 elevated; TSH
- Step 3: Cautious LT4+LT3 trial; reduce LT4 modestly; add LT3 2.5–5 mcg split dosing.
- Step 4: Monitor cardiac status, symptoms, and labs at 6–8 weeks.
- Step 5: If improved, maintain; if adverse, adjust or revert; sustain lifestyle momentum.
Mechanism-first care produces durable results without chasing a single lab value.
Ethical Practice—Navigating Polarized Messaging
Patients often encounter extremes: “TSH is everything” vs. “TSH is nothing.” My stance: TSH is important—but not sufficient in treated patients or complex physiology. I explain uncertainties, cite evidence, individualize care, and document decisions. Respecting both data and the person earns trust.
Research Horizons—Genomics, Tissue Biomarkers, and Slow-Release T3
The future of thyroid care:
- Genomics: Identify responders to combination therapy (e.g., DIO2 variants).
- Tissue biomarkers: Noninvasive proxies for intracellular T3 actions.
- Formulations: Slow-release T3 to mimic physiology.
- Systems medicine: Integrate thyroid metrics with metabolomics and microbiome data.
As these tools mature, current debates will fade. We are moving toward precise tissue-level readouts.
Practical Checklists For Thyroid Optimization
- Persisting symptoms despite normal TSH:
-
- Assess free T3, rT3, iron/ferritin, selenium, vitamin D, zinc, cortisol/sleep, insulin resistance, and inflammation.
- Optimize cofactors and lifestyle first.
- Consider cautious combination therapy if the mechanisms support it.
- Resistant weight:
-
- Screen for sleep apnea, insulin resistance, medication contributors, training adequacy, protein intake, and inflammation.
- Address sarcopenia with progressive resistance and protein sufficiency.
- Starting T3:
-
- Small doses, split dosing, reduce LT4, monitor cardiac/bone risk, reassess at 6–8 weeks.
Checklists keep teams aligned and decisions reproducible.
Timing Thyroid Labs—Why Standardization Is Non-Negotiable
When T3 is part of therapy, lab timing dictates interpretation:
- I standardize draws at 5–6 hours post-dose for DTE or combination therapy to avoid misreading early peaks.
- If a patient arrives 2 hours post-dose, I reschedule; peak levels do not represent steady-state exposure.
- For split dosing (e.g., 6 a.m., 12 p.m., 6 p.m.), I draw labs 5–6 hours after the morning dose for consistency.
This discipline turns random numbers into meaningful trends. It prevents reflexive dose changes based on peaks and improves patient safety.
Understanding T3 Peaks—Symptom Timing and Wearable Pulse Trends
Patients often report palpitations or jitteriness 1–2 hours post-dose. This aligns with T3 absorption and peak kinetics:
- I review wearable pulse data (e.g., from an Apple Watch) as a trend-tracking tool. Spikes near 2 hours are expected.
- If peaks are uncomfortable, I split doses or reduce the morning fraction, and review caffeine/stimulants near peak times.
- For sleep-sensitive patients, I move late doses earlier or reduce them to protect sleep architecture.
Managing peaks preserves benefits while minimizing side effects.
Free T3 Interpretation—Peaks Versus Mid-Day Plateaus
Interpreting free T3 requires context:
- 9 pg/mL at 2–3 hours post-dose typically indicates a peak; not inherently alarming without symptoms.
- 5–4.2 pg/mL mid-day often represents functional exposure. If fatigue persists at troughs, I redistribute dosing or consider modest adjustments.
I don’t chase peak values with dose cuts. I adjust splits to smooth the curve and align levels with the patient’s daily demands.
Ferritin and Iron—The Keystone of T4?T3 Conversion
I rarely succeed in optimizing thyroid therapy without first correcting iron. Ferritin is central to deiodinase activity and mitochondrial function:
- Low ferritin correlates with poor conversion, hair loss, fatigue, and exercise intolerance.
- I target ferritin thresholds (commonly 50–70 ng/mL as functional baselines, individualized) and treat iron deficiency with oral or IV strategies when needed.
- After iron repletion, patients often report improved energy, hair regrowth, and clearer cognition; free T3 rises and rT3
In practice, correcting iron is frequently the turning point.
Hashimoto’s—Split Dosing and Nutritional Supports
For Hashimoto’s, split dosing improves function:
- BID dosing (morning + early afternoon) sustains T3 across the day.
- Gluten reduction (for selected patients), selenium (100–200 mcg/day), zinc (15–30 mg/day), and careful iodine with selenium reduce inflammation and support conversion.
- Ferritin repletion and lab timing discipline reduce variability.
Hashimoto’s often requires slightly higher functional levels and tighter timing to stabilize daily energy and cognition.
Iodine Physiology—NIS Regulation and Halogen Competition
Iodine is foundational to thyroid and extra-thyroid tissues:
- The sodium-iodide symporter (NIS) transports iodide into cells; TSH can facilitate NIS expression.
- Halogens (bromine, chlorine, fluorine) compete at the receptor and transport steps; iodine saturation counteracts this burden.
- Western diets often deliver only microgram levels—sufficient to prevent goiter, not necessarily optimal physiology. Traditional Japanese diets typically fall within milligram ranges, though debates persist.
In practice, I titrate iodine carefully and pair it with selenium/zinc. TSH may rise transiently during repletion (transport remodeling). If free T3/T4 and clinical state improve, this transient shift is not pathologic. I closely monitor antibodies and clinical status in Hashimoto’s.
Cross-Tapering—From LT4 to Desiccated Thyroid
When transitioning from LT4 to DTE:
- Approximate equivalence: one grain (~60–65 mg) of DTE delivers ~38 mcg T4 and 9 mcg T3; functionally, one grain can align with 75–100 mcg LT4 for many.
- I initiate a two-week cross-taper: half the LT4 dose + half the DTE dose, then discontinue LT4 and continue the full DTE dose. This avoids abrupt changes and reduces jitteriness.
- I begin at 1–1.5 grains daily, reassess in 2–4 weeks, and adjust by 5-grain increments. BID dosing improves late-day function.
I avoid concurrent iron/calcium near dosing to protect absorption and lab interpretability.
Compounded T4/T3—Nature-Identical Ratios Without Porcine Products
For patients who prefer non-porcine options, compounded T4/T3 can approximate human ratios and reduce excipient exposure:
- I customize ratios to match conversion capacity and symptom patterns; increase the T3 fraction for poor converters and reduce it for jittery patients.
- TID helps pure T3; BID usually fits combination therapy.
- I rigorously standardize lab timing and document the off-label rationale, informed consent, and outcomes.
Customization aligns therapy with individual physiology.
Medication Choices—Synthroid, Levoxyl, Tirosint, and rT3 Considerations
LT4 formulations differ in excipients and absorption profiles. In poor converters, LT4 monotherapy often yields low free T3 and elevated rT3:
- If a patient thrives on LT4 alone—robust energy, normal free T3, low rT3—I leave therapy intact.
- If symptoms persist with low free T3/high rT3, I add LT3, transition to DTE, or compounded T4/T3, and correct iron, selenium, and zinc, and address sleep and stress.
The decision is not brand-driven; it is physiology-driven.
Psychiatric Interfaces—T3 Augmentation in Refractory Depression
Psychiatric literature supports T3 augmentation in refractory depression:
- T3 modulates neuronal transcription, synaptic plasticity, receptor density, and mitochondrial resilience.
- Trials show improved mood scores without consistent increases in osteoporosis or AFib when monitored carefully—even at doses higher than typical endocrine ranges.
In endocrine practice, we use lower doses and still see improvements in mood and cognition when free T3 is functionally low. Safety remains the priority.
Atrial Fibrillation Clarifications—Substrate Versus Hormone
I often hear that thyroid therapy “creates” AFib. Clarifications:
- AFib is rooted in electrical and structural substrate—fibrosis, atrial dilation, scarring, and ectopic foci.
- Over-replacement can exacerbate tachycardia; precision dosing and monitoring prevent this.
- In physiologic regimens, T3 supports cardiac performance without creating arrhythmia pathways; risk drivers remain age, OSA, hypertension, alcohol, electrolyte abnormalities, and structural disease.
I dose carefully and collaborate with cardiology. Context replaces fear with confidence.
Cardiometabolic Integration—Thyroid, Testosterone, Vitamin D/K2, Sleep, and Insulin
Outcomes improve when thyroid therapy operates within a systems framework:
- Thyroid: Optimize free T3 within safe, individualized targets.
- Testosterone/Estrogen/Progesterone: Correct deficiencies affecting muscle, vascular health, and cognition.
- Vitamin D/K2: Supports calcium handling, immune modulation, and endothelial function.
- Magnesium/Omega-3: Reduce inflammation and support electrophysiological stability.
- Sleep/OSA screening: Untreated OSA sabotages thyroid and cardiac function.
- Glycemic control: Stabilize insulin; hyperinsulinemia blunts deiodinase activity and worsens lipids.
- Exercise: Resistance + aerobic programming restores mitochondrial demand and conversion.
The synergy elevates resilience beyond what any single hormone delivers.
Pediatric, Adolescent, and Geriatric Considerations
Age matters:
- Adolescents require robust T3 signaling to fuel growth, myelination, and neurodevelopment. Upper-quartile free T3 may be physiologic and appropriate when vitals and clinical state are stable.
- Adults and older adults become more sensitive to T3 excess; titration must be conservative, with close monitoring for cardiac and sleep side effects.
- Pregnancy requires strict oversight; LT4 is traditionally favored, with specialist input for any deviations.
- Postpartum autoimmunity and iron deficits must be addressed to stabilize thyroid function.
I respect life-stage physiology to avoid over- or under-treatment.
Athletic Populations—Ferritin, T3 Availability, and Performance
Athletes often present with high energy demand, labile iron status, and conversion challenges:
- I replete ferritin, employ BID desiccated thyroid or LT4/LT3 split dosing, and refine nutrition and sleep.
- Outcomes: improved endurance, reduced post-exertional crashes, faster adaptation, and more stable training cycles.
Functional thyroid signaling is the difference between marginal and peak performance.
Women’s Health—Menses, Fertility, and Bone Integrity
Women with low T3 may experience:
- Heavy or irregular menses, PMS exacerbation.
- Infertility or luteal phase defects.
- Bone health concerns if hyperthyroidism is induced.
I maintain free hormone levels within physiologic ranges; I ensure iron sufficiency; I support with selenium, zinc, and careful iodine use; I monitor bone density in at-risk groups. Suppressed TSH alone, without signs of excess or supraphysiologic free hormones, does not mandate dose reduction.
Clinical Pearls—Day-to-Day Protocols That Prevent Errors
My practical rules:
- Always ask, “What time did you take your pill today?” before drawing labs.
- Standardize draws at 5–6 hours post-dose for T3-containing regimens.
- Split doses to manage peaks; reduce evening T3 for sleep-sensitive patients.
- Pair pulse trend data with symptoms and timing; use wearables as adjuncts, not diagnostic replacements.
These small practices prevent outsized mistakes.
Documentation—Off-Label Transparency and EMR Templates
When employing off-label approaches:
- I document symptoms, vitals, dosing, lab timing, and rationale, e.g., “Patient’s free T3 measured at 5.5 hours post-dose; improved energy; resting HR 72; peak HR 95 at ~2 hours per wearable; BP 118/72.”
- I record informed consent, safety parameters, and follow-up timelines.
- Consistent templates ensure reproducibility and ethical clarity.
Documentation is safety. It protects the patient and the team.
HealthVoice360 Case Stories—Standardization Unlocks Clarity
HealthVoice360.com carries narratives showing:
- Variable labs became coherent after the timing discipline was implemented.
- Afternoon crashes resolved with BID dosing and iron repletion.
- Insomnia improved when evening T3 was moved earlier or reduced.
- Patients’ confidence rose when physiology was explained, and protocols were transparent.
Case stories turn theory into lived successes.
Evidence Integration—Mechanistic, Clinical, and Real-World Data
I synthesize:
- Mechanistic studies of deiodinases and transporter biology.
- Clinical trials comparing monotherapy versus combination therapy outcomes.
- Real-world cohort data (e.g., thyroid cancer survivors on suppression) clarifying safety.
- Observational outcomes from routine practice are aligned with standardized lab timing and functional metrics.
Evidence-based medicine thrives when these streams converge.
Quality Improvement—Embedding Precision in Clinic Workflows
We audit:
- Lab timing adherence.
- Dose-adjustment outcomes.
- Patient-reported measures (energy, sleep, cognition).
We train staff on pharmacokinetics and safety, implement EMR templates, and create automated reminders for lab timing. Precision becomes habit; habits produce reliable care.
Systems Medicine View—Thyroid Care As Network Optimization
Thyroid care is not a gland-only enterprise. It is network optimization:
- Endocrine axes (thyroid, adrenal, gonadal) converge in mitochondria and receptor signaling.
- Metabolic regulators (insulin, inflammation) modulate deiodinases and receptor coactivators.
- Sleep and the autonomic nervous system create the rhythm for hormone release; training provides the stimulus; nutrition provides the substrate.
Aligning these systems yields durable recovery in energy, cognition, metabolism, and quality of life.
Summary
This educational post explains, in a first-person narrative, why thyroid care must move beyond TSH-only thinking, especially in treated patients. I show how tissue-level thyroid action—transport, conversion, receptor binding, and mitochondrial execution—is governed by free T3 and modulated by the balance of deiodinases (DIO1/DIO2/DIO3), inflammation, stress, micronutrients, and sleep. I detail why LT4 monotherapy can leave a subset symptomatic and how carefully executed LT4+LT3 or DTE therapy, with strict lab timing (5–6 hours post-dose), split dosing, iron/ferritin repletion, and selenium/zinc support, can restore function safely. I integrate metabolic care—insulin sensitivity, resistance training, Zone 2 aerobic work, sleep optimization—and endocrine cross-talk (testosterone, estrogen/progesterone) to clarify how systems medicine transforms outcomes.
I describe dosing and monitoring guardrails, explain the physiology of T3 peaks and how wearables inform timing, and illustrate why suppressed TSH under therapy must be interpreted in context with free hormone levels, vitals, and patient function. Real-world cases from HealthVoice360.com align with these principles, demonstrating that standardization, communication, and mechanism-first protocols yield predictable improvements. Throughout, I anchor techniques in modern evidence-based research and leading investigator findings, showing how mechanistic insights translate into compassionate, individualized care.
Conclusion
Modern thyroid care succeeds when we honor mechanisms, personalize therapy, and embed safety through timing discipline and collaborative monitoring. Free T3 drives tissue-level action; TSH is valuable for screening but insufficient to judge treated physiology. A subset of patients requires T3-inclusive strategies—implemented with split dosing, iron and micronutrient support, anti-inflammatory nutrition, exercise, sleep restoration, and cross-axis optimization—to convert laboratory normalization into lived well-being. By committing to standardized lab timing, mechanistic diagnostics, and stepwise algorithms, we minimize risk and elevate outcomes. The field is moving toward genomics, tissue biomarkers, and improved formulations, but the core remains: evidence-informed, patient-centered, physiology-first care.
Key Insights
- TSH is an upstream screening signal; it does not guarantee normal tissue T3 action in treated patients.
- Free T3 often correlates best with function; deiodinase balance (DIO1/DIO2/DIO3), inflammation, stress, and micronutrients determine conversion.
- LT4 monotherapy can leave a subset symptomatic; cautious LT4+LT3 or DTE therapy, with strict lab timing and split dosing, restores tissue T3 safely.
- Standardize lab draws at 5–6 hours post-dose for T3-containing regimens to avoid misinterpreting peaks and to create comparable trends.
- Correct iron/ferritin, selenium, zinc, and vitamin D before escalating doses; fix sleep apnea, improve insulin sensitivity, and build lean mass.
- Interpret suppressed TSH in context: free hormones, vitals, symptoms, and safety metrics matter more than the pituitary’s solitary voice.
- Integrate thyroid therapy with metabolic care, sex hormone balance, sleep, nutrition, and exercise for durable outcomes.
- Document off-label rationale, informed consent, and standardized monitoring in the EMR; use wearables as trend adjuncts.
- Employ stepwise algorithms and mechanism-first reasoning to minimize risk and personalize dosing.
- Future advances—genomics, tissue biomarkers, slow-release T3—will refine targeting, but disciplined, individualized care is effective now.
References
- Hoermann R, Midgley JE, Larisch R, Dietrich JW. Homeostatic control of the thyroid-pituitary axis: Perspectives for diagnosis and treatment. Front Endocrinol (Lausanne).
- Jonklaas J, Bianco AC, Bauer AJ, et al. Guidelines for the treatment of hypothyroidism. Thyroid.
- Escobar-Morreale HF, Botella-Carretero JI, Gómez-Bueno M, et al. Thyroid hormone replacement therapy in primary hypothyroidism: A randomized trial comparing L-thyroxine alone versus combination therapy with L-thyroxine and L-triiodothyronine.
- Wiersinga WM. Paradigm shifts in thyroid hormone replacement therapies. Nat Rev Endocrinol.
- Peeters RP. Subclinical hypothyroidism. N Engl J Med.
- Silva JE. Thermogenic mechanisms and their hormonal regulation. Physiol Rev.
- Clinical observations and educational resources by Dr. Alexander Jimenez, DC, APRN, FNP-BC.
- Contemporary endocrinology literature on deiodinase activity, transporter biology, and combination therapy outcomes.
- Cardiometabolic and critical care studies linking low free T3 with outcomes in heart failure, myocardial infarction, ARDS, and sepsis.
- Memory clinic studies on free T3 and progression from mild cognitive impairment to Alzheimer’s disease.
- Psychiatry literature on T3 augmentation in depression and mood disorders.
Keywords: hypothyroidism, levothyroxine, liothyronine, desiccated thyroid extract, TSH, free T3, reverse T3, deiodinase, DIO1, DIO2, DIO3, DIO2 polymorphism, thyroid autoimmunity, selenium, iron, ferritin, zinc, insulin resistance, mitochondrial function, testosterone, SHBG, obesity, resistance training, Zone 2, sleep apnea, evidence-based thyroid care, lab timing, pharmacokinetics, dose splitting, atrial fibrillation, osteoporosis, HealthVoice360
Disclaimer: The information provided in this educational post is for informational purposes only and is not medical advice. It should not be used to diagnose, treat, cure, or prevent any disease.
Additional Disclaimer: Every individual’s health situation is unique. All individuals must obtain recommendations for their personal situations from their own qualified healthcare providers.
General Disclaimer
Professional Scope of Practice *
The information herein on "Thyroid Optimization: Your Guide to Balanced Hormones" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multistate
Multistate Compact RN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
RN: Registered Nurse
APRNP: Advanced Practice Registered Nurse
FNP: Family Practice Specialization
DC: Doctor of Chiropractic
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics